If you have noticed tissue bulging from the anus during a bowel movement or after straining, then seeming to improve later, you may be wondering whether prolapsed hemorrhoids can come and go. The short answer is yes. Symptoms of prolapsed hemorrhoids often flare up and calm down over time, especially in the earlier stages.
That does not always mean the problem is gone. Hemorrhoids may continue to enlarge, become more symptomatic, or prolapse more often if the underlying pressure and irritation are not addressed.
What Is a Prolapsed Hemorrhoid?
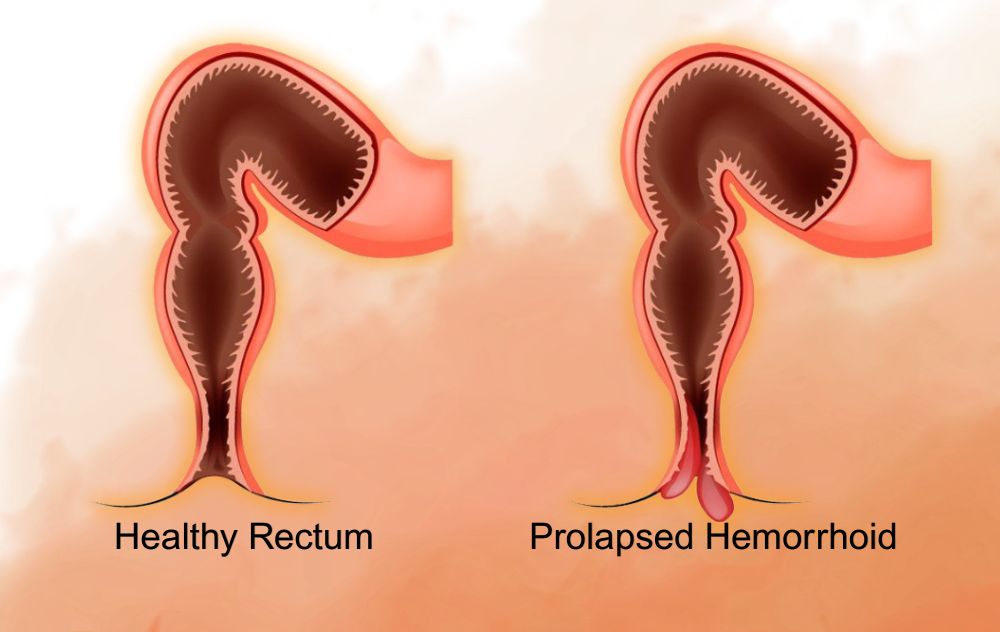
A prolapsed hemorrhoid happens when swollen internal hemorrhoid tissue stretches downward and protrudes outside the anal opening. Internal hemorrhoids develop inside the rectum, but as they enlarge, they can slip outward during bowel movements or straining.
Unlike external hemorrhoids, internal hemorrhoids may not always be painful, but prolapse can lead to irritation, mucus leakage, itching, pressure, and discomfort.
Learn More About Prolapsed Hemorrhoids
Prolapsed Hemorrhoids Can Come and Go
In many cases, prolapsed hemorrhoids are not always visible. Symptoms may appear during flare-ups and improve afterward.
You may notice that the hemorrhoid:
- Comes out during bowel movements
- Goes back in on its own
- Needs to be gently pushed back in
- Feels worse after constipation or prolonged sitting
- Improves when swelling decreases
This pattern is common because hemorrhoid symptoms often change based on inflammation, pressure, bowel habits, and irritation in the area.
Why Do Prolapsed Hemorrhoids Flare Up?
Several factors can increase pressure in the rectal veins and make prolapse more noticeable.
Common triggers include:
- Constipation
- Straining during bowel movements
- Sitting on the toilet too long
- Chronic diarrhea
- Pregnancy
- Heavy lifting
- Obesity
- Low-fiber diet
- Long periods of sitting
Even if symptoms improve between flare-ups, repeated pressure can cause hemorrhoids to worsen over time.
Find a Hemorrhoid Center Near You
Grades of Prolapsed Hemorrhoids
Healthcare providers often classify internal hemorrhoids by how much they prolapse:
Grade I
No prolapse. Internal hemorrhoids remain inside the rectum.
Grade II
The hemorrhoid prolapses during bowel movements but goes back in on its own.
Grade III
The prolapsed hemorrhoid needs to be manually pushed back inside.
Grade IV
The hemorrhoid remains prolapsed and cannot be pushed back in.
As the hemorrhoid grade increases, symptoms may become more persistent and harder to manage with home care alone.
Symptoms That May Come and Go
Many people experience intermittent symptoms such as:
- Bright red bleeding during bowel movements
- Itching
- Swelling
- A feeling of fullness
- Mucus leakage
- Irritation
- Tissue protruding during bowel movements
- Discomfort when sitting
These symptoms may ease temporarily, then return during the next flare-up.
Can Prolapsed Hemorrhoids Heal on Their Own?
Mild prolapse may improve when swelling goes down and bowel habits improve. However, hemorrhoids do not always fully resolve without addressing the cause of repeated pressure.
That is why symptoms may seem better for a while, then return later.
What Can Help Reduce Flare-Ups?
Conservative care may help manage symptoms and reduce irritation:
- Increase fiber intake
- Drink more water
- Avoid straining
- Limit time on the toilet
- Stay physically active
- Use warm sitz baths
- Avoid prolonged sitting when possible
These steps may help, but they may not correct larger or recurring prolapsed hemorrhoids.
When to See a Specialist
You should seek medical attention for hemorrhoids if you have:
- Frequent bleeding
- Recurrent prolapse
- Pain or severe discomfort
- Trouble cleaning the area
- Symptoms that keep returning
- Uncertainty whether it is hemorrhoids or another condition
Rectal bleeding and anal lumps can have causes other than hemorrhoids, so an accurate diagnosis matters.
Diagnosis and Treatment Options for Prolapsed Hemorrhoids
A specialist can diagnose prolapsed hemorrhoids through a medical history, symptom review, and physical examination. In some cases, additional evaluation may be recommended to rule out other causes of bleeding or rectal symptoms.
Treatment depends on the type of hemorrhoid, severity of prolapse, bleeding, and how often symptoms return. Options may include lifestyle changes, office-based procedures, or advanced treatment for internal hemorrhoids.
For eligible patients with symptomatic internal hemorrhoids, hemorrhoid artery embolization is a minimally invasive outpatient procedure that reduces blood flow to the hemorrhoidal tissue. This may help improve bleeding and hemorrhoid symptoms without surgical removal. It is typically considered for internal hemorrhoids rather than external hemorrhoids.
Get Evaluated at USA Hemorrhoid Centers
If prolapsed hemorrhoids keep coming back or symptoms are affecting your daily life, an evaluation can help identify the cause and review your treatment options. USA Hemorrhoid Centers offers non-surgical evaluations and advanced treatment options for eligible patients.
FAQs About Prolapsed Hemorrhoids
Yes. Some prolapsed hemorrhoids retract on their own, while others may need gentle manual reduction.
Straining and increased pressure during bowel movements can push swollen internal hemorrhoid tissue outward.
Not always. Some are intermittent, but repeated prolapse can become more persistent over time.
