With external hemorrhoids, many sufferers turn to self-care options as the go-to for addressing itching, swelling, and discomfort. While some use topical creams or sitz baths, others use witch hazel pads as a natural remedy.
Natural remedies for hemorrhoids, while they help some people, may not provide the immediate relief that many seek. Those who deal with hemorrhoids that persist for months often wonder if remedies like witch hazel wipes or pads can be left on overnight for more effective relief.
In short, prolonged use of witch hazel pads may not help resolve hemorrhoids because they only treat the surface. While witch hazel can soothe external skin, they cannot reach internal hemorrhoids or address the underlying blood flow issues that cause hemorrhoids to swell. Understanding these limitations is the first step toward exploring medical options that provide deeper, more lasting relief.
Understanding Hemorrhoid Types
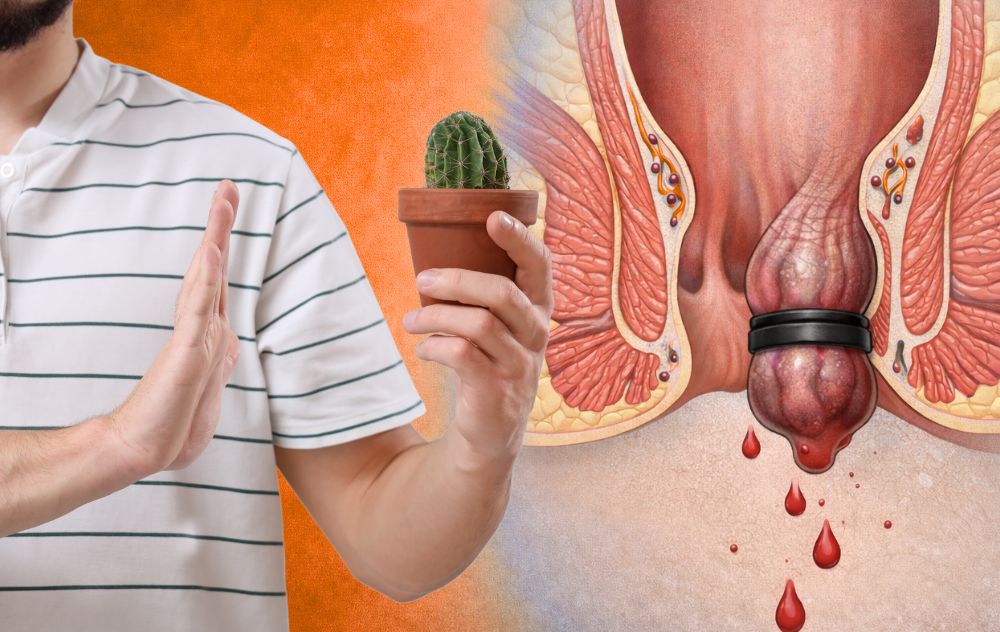
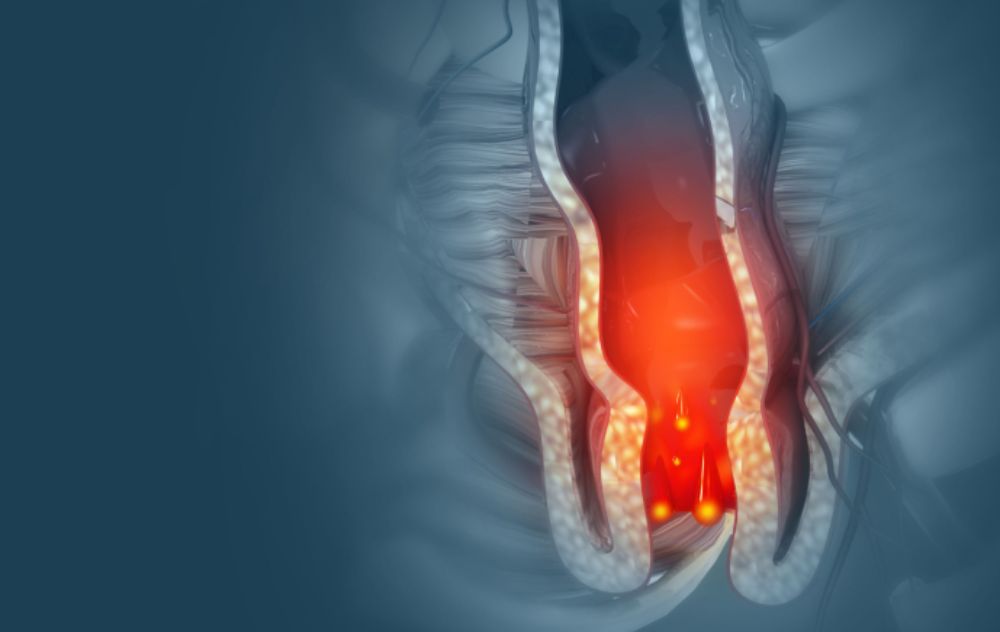
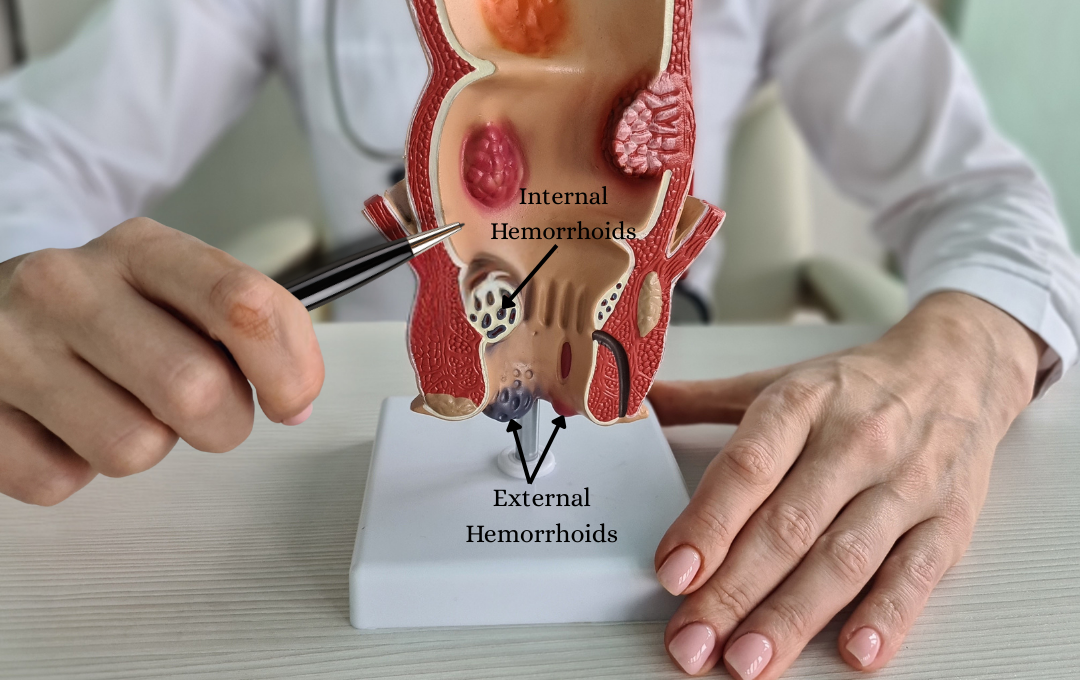
Hemorrhoids are swollen veins in or around the rectum and anus. Hemorrhoids that develop underneath the skin around the anus are called external hemorrhoids, which may cause painful irritation or itching. Hemorrhoids that form inside the rectum are classified as internal hemorrhoids, which cause bleeding or feelings of fullness, even after bowel movements. Many patients suffer from both types simultaneously, but the intense itching and pain from external hemorrhoids can often mask the presence of internal ones.
Overview of Witch Hazel

Witch hazel is a plant-derived tincture with various self-care uses, including skincare, minor wound healing, and hemorrhoids. While there are various plant species, one type, Hamamelis virginiana, has been used in alternative medicine for centuries. Today, it is widely available in liquid form, wipes, and medicated pads at pharmacies and drugstores.
What Is Witch Hazel Good For?
Witch hazel is classified as an astringent, meaning that it shrinks tissues to reduce inflammation and irritation. This may temporarily relieve discomfort associated with hemorrhoids.
Aside from hemorrhoids, witch hazel is often used for skincare, toning, acne, dandruff, and minor injuries, such as bruises, small cuts, and bug bites. While many in the alternative medicine community praise witch hazel’s versatile uses, there is little research to support its health benefits.
Witch Hazel Pads and Hemorrhoids
Witch hazel’s anti-inflammatory properties are especially appealing to patients with hemorrhoids. However, while witch hazel pads are primarily used for external hemorrhoids, it can irritate the inner lining of the rectum.
Are Witch Hazel Pads Good for Hemorrhoids?
Witch hazel pads for hemorrhoids may help reduce itching, mild pain, and inflammation, especially for external hemorrhoids. However, the effects are typically short-lived and will not completely resolve hemorrhoids. Additionally, witch hazel pads that contain alcohol may cause temporary stinging when applied to sensitive skin.
For some patients with internal hemorrhoids, witch hazel pads may not help at all, and their symptoms will continue to worsen until the internal hemorrhoid .
How to Use Witch Hazel on Hemorrhoids

There are multiple ways to apply witch hazel to hemorrhoids. Witch hazel pads can be convenient, but some may prefer to soak a cotton ball in the tincture before applying or add it to a warm sitz bath. Regardless of how it’s applied, it’s recommended to apply witch hazel after bowel movements or as needed throughout the day. The area should be gently cleaned and patted dry before use. Avoid rubbing during the application, as this may worsen irritation.
Should You Leave Witch Hazel Pads on a Hemorrhoid Overnight?
While short-term contact is safe, many witch hazel pads contain isopropyl alcohol, which can irritate or dry the skin during prolonged use. If using witch hazel pads for hemorrhoids, carefully read the instructions to avoid the potential side effects.
When to See a Doctor

Witch hazel pads should be used only as a temporary measure. It’s advised to seek medical attention if you experience:
- Rectal bleeding that persists or worsens.
- Severe pain or swelling.
- Symptoms lasting longer than one week.
- New irritation after applying.
Persistent symptoms may require evaluation beyond natural remedies for hemorrhoids.
Alternative Treatments for Hemorrhoids
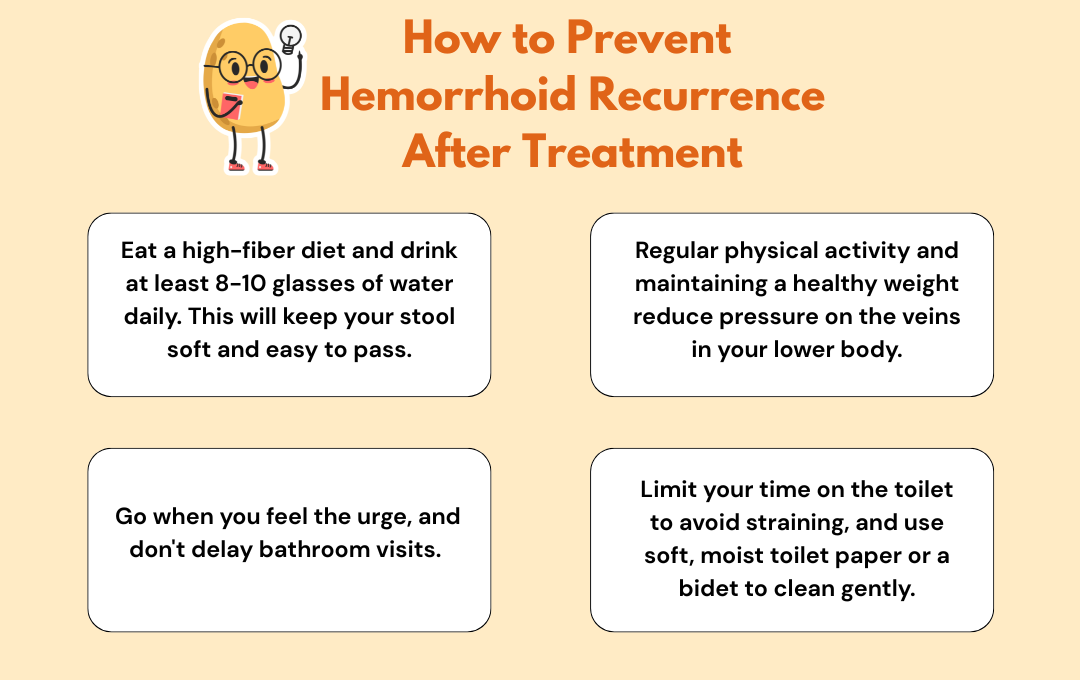
There are other home remedies for hemorrhoids that some patients may try before seeking medical help. This can include aloe vera, warm sitz baths, increasing fiber and water intake, and avoiding straining during bowel movements. While these self-care methods can provide temporary relief, they aren’t a permanent fix. If your symptoms persist or worsen despite home remedies, it may be time to consider a medical procedure for a more lasting solution.
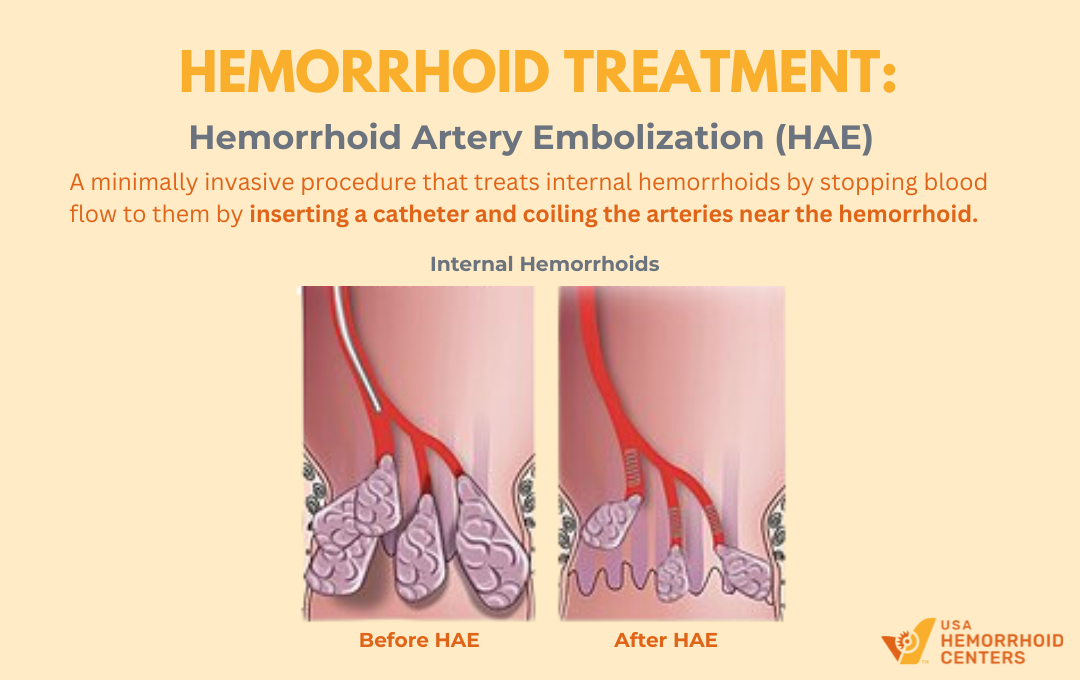
Hemorrhoid Artery Embolization: A Revolutionary Game-Changer
For individuals with recurrent or severe internal hemorrhoids, minimally invasive procedures such as hemorrhoid artery embolization (HAE) may be considered. HAE works by reducing blood flow to hemorrhoidal tissue, causing the swollen hemorrhoids to shrink and stop bleeding.
Traditionally, patients who have relied on topical creams and witch hazel pads with little to no relief were offered surgery to remove the hemorrhoid. Some may also be recommended procedures, such as rubber band ligation. While these procedures may help, the recovery can be long and painful. HAE offers an alternative to these procedures, with minimal risk and side effects and shorter recovery times.
At USA Hemorrhoid Centers, our specialists focus on diagnosing the type and severity of hemorrhoids and guiding patients toward treatment options that address the underlying cause—not just the symptoms. For many, this clarity is the turning point after months or even years of managing flare-ups on their own.
Persistent pain, bleeding, or discomfort is not something patients have to live with, and expert evaluation can help determine whether minimally invasive treatment is the right next step.
If you are ready to find effective relief from hemorrhoids, schedule a consultation to get started.