Many people find that when it comes to hemorrhoids, a high-fiber diet is vital to preventing and easing uncomfortable symptoms. Fiber supports digestive health by softening stool and promoting regular bowel movements, reducing the strain that can cause swollen or irritated veins in the rectal area. For most patients, a fiber-rich diet can help improve symptoms. However, fiber is not a one-size-fits-all solution; hemorrhoid relief is most effective when a healthy diet is paired with targeted medical treatment.
While many foods contain fiber, some are particularly effective for those managing hemorrhoid symptoms. Choosing a diet for hemorrhoids that includes a mixture of fruits, vegetables, grains, and legumes means you can find relief naturally while supporting overall digestive health.
How Fiber Supports Hemorrhoid Relief
A high-fiber diet offers various benefits for digestion and short-term relief of hemorrhoid symptoms. It’s one of the most effective natural ways to prevent hemorrhoids because it helps keep the digestive system moving smoothly.
When you consume enough fiber, stools become softer and easier to pass, reducing pressure on rectal veins, which is a leading cause of hemorrhoids. Softer stools mean less straining, which minimizes irritation, swelling, and bleeding, which is especially valuable for internal hemorrhoids.
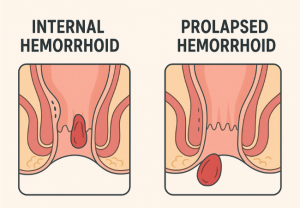
A high-fiber diet is particularly beneficial for mild hemorrhoids or recurring symptoms. However, dietary changes may not be enough for severe cases such as prolapsed or bleeding hemorrhoids, which often require medical intervention. If you are experiencing symptomatic hemorrhoids and are looking for relief, it is recommended to consult with a specialist to explore treatment options.
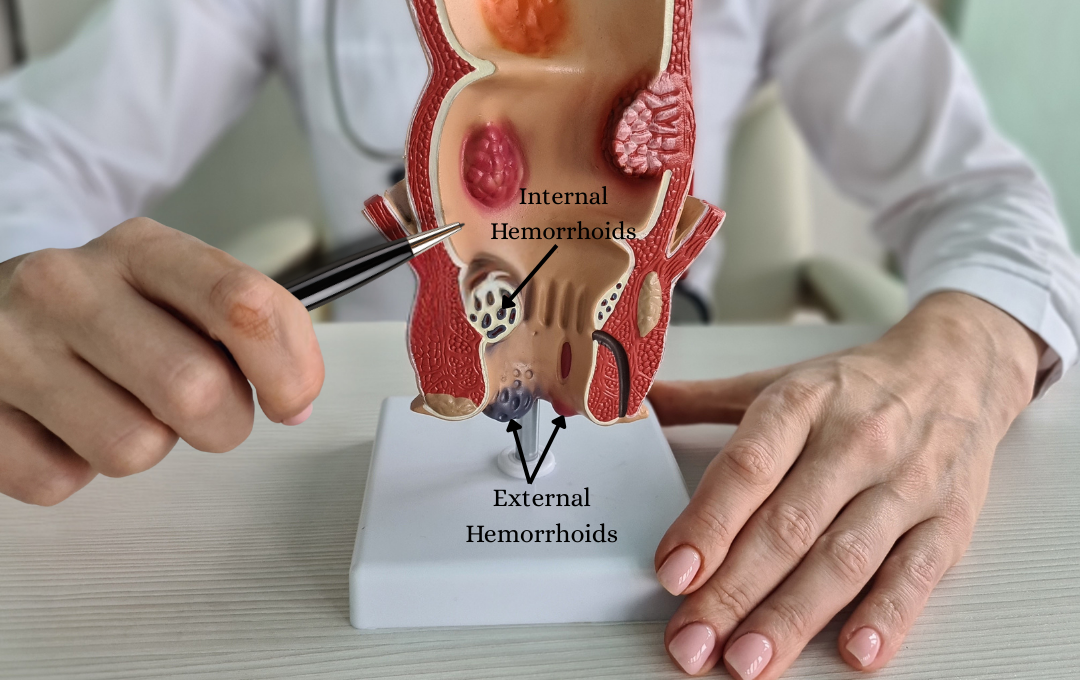
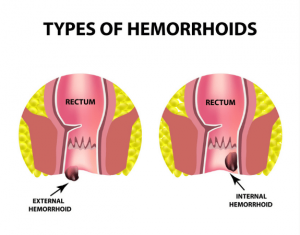
Fiber and Internal Hemorrhoids
Internal hemorrhoids are inside the rectum and often linked to poor bowel habits. When stool is difficult to pass, it puts extra strain on these veins, leading to pain, swelling, and occasional bleeding.
With hemorrhoids, a consistent, high-fiber diet can minimize issues by promoting softer stools and more regular bowel movements. People who maintain steady fiber intake throughout the day tend to experience fewer flare-ups and greater long-term relief.
Best High Fiber Foods for Hemorrhoids
Not all fiber-rich foods are created equal. When it comes to a high-fiber diet and hemorrhoids, here are some of the best sources to prevent and manage symptoms.1
Five Best Fiber-Rich Fruits
- Apples: Rich in both soluble and insoluble fiber, eating one apple a day adds over 4g of fiber to your diet while promoting digestive regularity.
- Pears: Excellent for a high-fiber diet and managing hemorrhoids, as one medium pear contains almost 6g of fiber along with pectin, a soluble fiber that helps maintain a softer stool consistency.
- Berries: Eating half a cup of berries means you get between 3g and 4g of insoluble fiber, along with antioxidants that can help reduce inflammation.
- Prunes: These natural laxatives help prevent constipation and straining, and a ¼ cup of prunes adds about 3g of fiber to your diet.
- Kiwi: A ½ cup of kiwis adds over 2g of fiber, and they contain actinidin, an enzyme that helps improve bowel movement frequency.
Three Best Vegetables To Improve Gut Health
- Broccoli: Packed with over 5g of fiber per cooked cup, broccoli also provides additional nutrients that support digestion.
- Leafy greens: Greens like spinach and kale, which both contain over 4g of protein per cup when cooked, are gentle on the digestive system and rich in magnesium, which aids regularity.
- Sweet potatoes and potatoes: Eating both regular and sweet potatoes adds 3-7g of fiber to your diet, along with complex carbohydrates.
Top Three Whole Grains
- Oat bran: A ¼ cup contains 1.5g of soluble fiber, which forms a gel-like consistency to soften stool.
- Whole Wheat Roti: While traditional roti made with whole wheat flour provides plenty of fiber (1.4g per ½ oz), you can also make roti with other ingredients, such as chickpeas, which are a good, fiber-rich, gluten-free alternative.
- Barley: A ¼ cup of pearled, cooked barley helps feed beneficial gut bacteria that aid digestion, while also adding 1.5g of fiber to your diet.
Best Legumes (Beans)
- Lentils: This fiber powerhouse adds almost 4g of fiber per ¼ cup when cooked, helping promote regular bowel movements so you strain less and reduce your risk of hemorrhoids.
- Chickpeas: Around ¼ cup of cooked chickpeas adds over 3g of soluble and insoluble fiber for balanced digestion.
- Black beans: Contain resistant starch, which supports a healthy gut microbiome, with a ¼ cup of cooked black beans adding around 4g of fiber.
Foods to Avoid
Although there are lots of good high-fiber foods for hemorrhoids, there are certain foods that can worsen symptoms by causing constipation, inflammation, or poor digestion.
These foods include:
- Processed foods
- Red meat
- Sugary foods
- Dairy
Red meat and dairy specifically exacerbate hemorrhoids as they are low in fiber and can cause digestive issues like constipation. These foods, along with processed and sugary foods, are also high in fat, which can slow digestion and lead to straining during bowel movements. The straining irritates and places pressure on the veins around the anus and rectum, which can lead to hemorrhoids.
How Much Fiber Do You Need for Hemorrhoid Relief?

Doctors and other medical specialists often recommend aiming for 28 grams of fiber per day from food sources.2 Most people fall short of this goal, but focusing on high fiber foods for hemorrhoids, also known as piles, is necessary to keep the digestive system moving smoothly and reduce irritation.
To improve your fiber intake for hemorrhoids, gradually increase it to help prevent bloating and gas. It’s also helpful to drink plenty of water, since fiber is most effective when you’re hydrated. If you’re struggling to increase fiber intake, fiber supplements can help when taken alongside a fiber-rich diet.
When Fiber Isn’t Enough: Seeking Hemorrhoid Treatment
Increasing fiber for hemorrhoids is one of the simplest and most effective lifestyle changes to support bowel health and prevent straining. While a high-fiber diet is a good first step for managing hemorrhoids, some cases require more than dietary changes. Severe hemorrhoids, such as those that are prolapsed or bleeding, often need medical treatment.
Our expert specialists at USA Hemorrhoid Centers use hemorrhoid artery embolization (HAE), a minimally invasive procedure specifically for treating internal hemorrhoids.
HAE targets the blood supply feeding the hemorrhoid, causing it to shrink and relieving symptoms such as pain, itching, and bleeding. Compared to dietary adjustments, HAE provides faster, lasting relief and does not require surgery or extended recovery time.
USA Hemorrhoid Centers Is Here to Help
While dietary improvements are an excellent first step, moderate to severe hemorrhoids often require professional care. USA Hemorrhoid Centers’ specialized, patient-focused treatment for internal hemorrhoids can help you when lifestyle and dietary changes aren’t enough. Our accredited nationwide clinics mean you have access to our specialists no matter where you live in the United States.
Don’t let hemorrhoids interfere with your life. A high-fiber diet can make a big difference, but if symptoms persist, schedule a consultation with USA Hemorrhoid Centers to learn more about your treatment options.
FAQs About a High Fiber Diet and Hemorrhoids
The fastest treatment for shrinking hemorrhoids is non-surgical treatments like hemorrhoid artery embolization (HAE). This minimally invasive procedure blocks the arteries that supply blood to the hemorrhoids, causing them to shrink gradually.
When increasing fiber intake for managing hemorrhoids, it can take anywhere from a few days to a week to start noticing results. More advanced cases of hemorrhoids may require medical intervention to improve symptoms.
If your hemorrhoids persist or get worse after focusing on a high-fiber diet, consult a medical professional to see if treatment options such as hemorrhoid artery embolization (HAE) can be effective.
Sources
- “Current Dietary Guidelines,” Food Sources of Dietary Fiber | Dietary Guidelines for Americans.
- “Interactive Nutrition Facts Label,” Interactive Nutrition Facts Label.