If you’ve been struggling with persistent hemorrhoid symptoms, you may be googling other treatment options that could help alleviate rectal bleeding and swelling because self-care methods haven’t worked. You may have heard about hemorrhoid artery embolization (HAE), a minimally invasive treatment that’s gaining recognition as an alternative to surgery. While HAE is proven to effectively reduce symptoms, many are unaware of how this procedure works and whether it’s right for them.
This blog will provide a clear explanation of how HAE works and how it differs from other medical procedures. Whether you’re seeking relief from stubborn hemorrhoids or simply weighing your options, staying informed of treatment options can help you determine what will be best for you.
Why Do Patients Need A Hemorrhoid Artery Embolization?
Patients typically need HAE when their hemorrhoids are causing persistent and bothersome symptoms that haven’t responded well to other treatments.
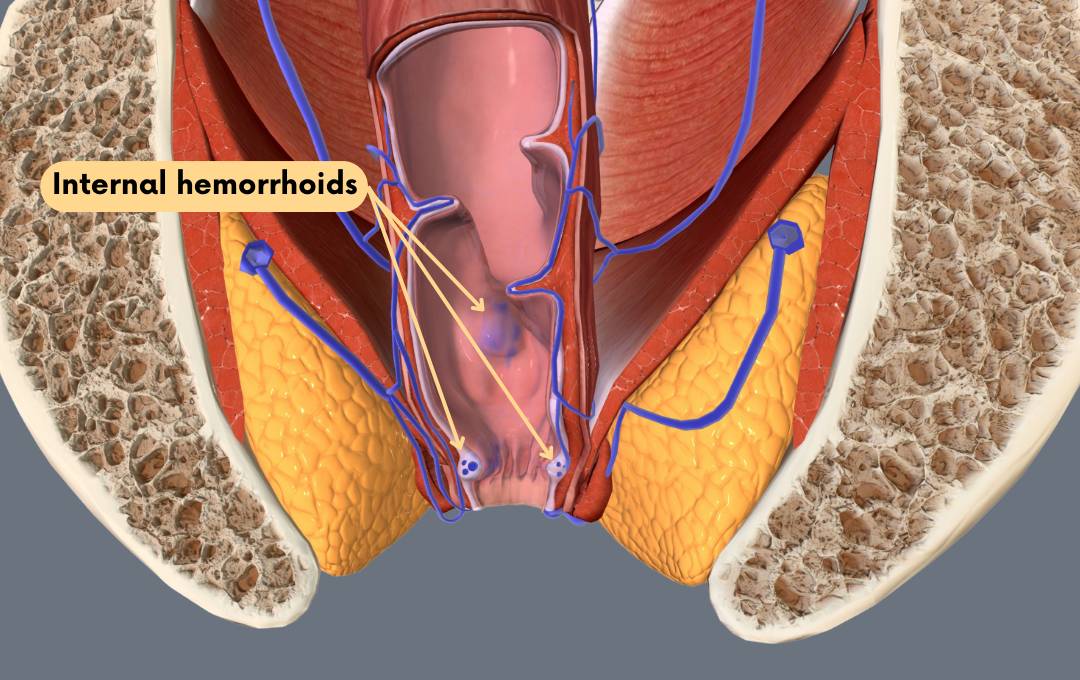
HAE is primarily used on internal hemorrhoids, especially those classified as Grade 1, 2, or 3. These grades typically refer to the extent of prolapse (how much they bulge outside the anus).
One of the most common and distressing reasons patients seek HAE is chronic or recurrent rectal bleeding from their hemorrhoids. This bleeding can range from minor spotting to significant blood loss, sometimes leading to anemia. HAE effectively targets the blood supply to these hemorrhoids, cutting off the flow and stopping the bleeding.
Traditional surgical hemorrhoidectomy, while effective, is known for being painful and having a prolonged recovery period. Many patients are unwilling or unable to undergo such an invasive procedure.
Some patients may not be suitable candidates for other common minimally invasive office-based procedures like rubber band ligation, sclerotherapy, or infrared photocoagulation due to the nature or severity of their hemorrhoids, or due to other medical conditions. HAE offers an alternative for these individuals.
What is Hemorrhoid Artery Embolization?
HAE is a minimally invasive procedure that reduces blood flow to internal hemorrhoids to resolve bleeding, swelling, and other hemorrhoid symptoms. Internal hemorrhoids form inside the rectum, but if they are untreated, they can eventually prolapse and cause significant pain and discomfort.
HAE is done by an interventional radiologist, which is a doctor who uses medical imaging equipment and catheters to treat various conditions from varicose veins to liver cancer. This targeted approach offers fewer risks, has a shorter recovery time, and is more cost-effective than surgery.
How Does HAE Work?
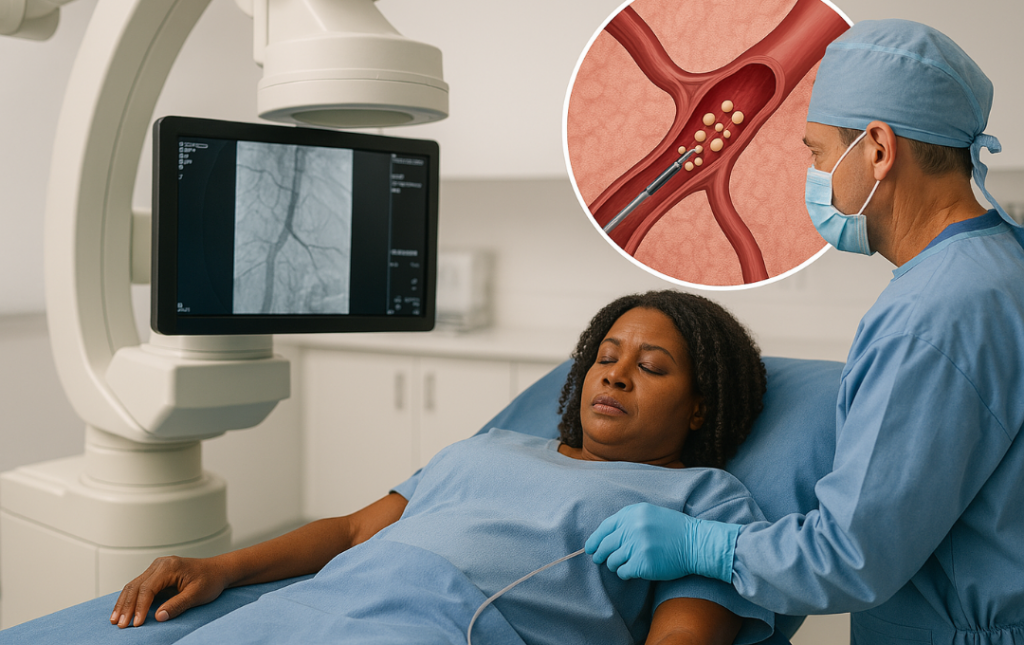
Prior to HAE, patients are given a light sedative for a painless experience. Once the sedation sets in, the interventional radiologist will insert a tiny catheter into an artery in the wrist or groin. Using an ultrasound, the catheter is guided to the rectal artery that supplies blood to the hemorrhoid.
Once the catheter is near the hemorrhoid, tiny particles called embolization agents are injected into the hemorrhoidal arteries. Patients very rarely experience side effects from these particles, which have been used in other FDA-approved procedures for over 30 years.
Patients leave with a small adhesive bandage over the insertion site after their HAE treatment. Most daily activities can resume within a few days. Over the next few weeks, the hemorrhoid will shrink, and patients will notice a significant improvement.
How Long Does Hemorrhoid Artery Embolization Last?
Current research on HAE shows that treatment benefits can last more than a year after treatment. Most patients report satisfaction with the results and have a lower risk of flare-ups compared to other procedures. One study from the Journal of Vascular and Interventional Radiology notes that in a sample size of 133 patients, only 10 of them needed a second procedure because of recurrent flare-ups post-procedure.
What Can I Do to Prevent Hemorrhoids from Coming Back?
There is always a risk of hemorrhoid symptoms coming back after treatment. Addressing risk factors that worsen hemorrhoids can help prevent symptoms from coming back. This can be achieved by:
- Using laxatives to avoid constipation
- Adding more fiber to your diet
- Staying active and making movement throughout your day
- Maintaining a healthy BMI
What is the Success Rate of Hemorrhoid Artery Embolization?
HAE has a clinical success rate of up to 95% with minimal side effects, according to Endovascular Today. This is apparent in cases like Susan Duarte’s HAE treatment at USA Hemorrhoid Centers’ Vienna, VA clinic.
“I recently underwent a nonsurgical procedure that provided better results than the surgeries I already had to address the issues,” said Susan.
While other procedures like rubber band ligation or surgery can help alleviate symptoms, many patients are still at risk of their hemorrhoid symptoms returning. Below is a table illustrating the effectiveness of different hemorrhoid procedures.
| Procedure | Success Rate | Rate of Recurrence | Pain/Recovery |
|---|---|---|---|
| Hemorrhoid artery embolization | 95% | Low | Mild |
| Rubber band ligation | 70-90% | Moderate | Mild |
| Hemorrhoid removal surgery (hemorrhoidectomy) | 95-98% | Low | High |
| Hemorrhoid repositioning (stapled hemorrhoidopexy) | 80-90% | Moderate | Moderate |
| Infrared coagulation (heating hemorrhoidal blood vessels) | 60-80% | High | Minimal |
Is Hemorrhoid Artery Embolization Painful?
HAE is virtually painless because of how the treatment is performed. Light sedation can help minimize discomfort during the procedure, and since no incisions are involved, the risk of pain post-treatment is significantly lower than surgery.
Susan Duarte said she was pleasantly surprised by how painless her HAE treatment was.
“The procedure was comfortable with minimal downtime, and I noticed positive results quickly,” she said.
Hemorrhoid Artery Embolization at USA Hemorrhoid Centers
USA Hemorrhoid Centers understand that persistent hemorrhoid symptoms can be painful as they are embarrassing. As an outpatient provider nationally recognized by the Accreditation Association for Ambulatory Health Care (AAAHC), we ensure our patients receive the best hemorrhoid care.
Reflecting on her experience, Susan Duarte spoke about the patient-focused care she received from USA Hemorrhoid Centers:
“Dr. Taghipour walked me through each step and answered all my questions,” said Susan. “The nurses provided attentive, personalized care. I highly recommend this non-surgical option and Dr. Taghipour’s practice to anyone with similar concerns.”
With over 25 locations in New York, Texas, Maryland, Virginia, New Jersey, Pennsylvania, and Washington, D.C., USA Hemorrhoid Centers provides evidence-based care to help you get back to enjoying life with fewer disruptions. They also accept most health insurance plans.
If you’re still unsure whether HAE is right for you, schedule a consultation with one of our specialists today for more information.