Hemorrhoids are a common condition, but many people don’t realize how they can progress over time. If you’ve been diagnosed with internal hemorrhoids—or suspect you may have them—you might be wondering: can internal hemorrhoids turn into prolapsed hemorrhoids?
The short answer is yes. Without proper diagnosis and treatment, internal hemorrhoids can worsen and eventually prolapse, leading to more noticeable symptoms and discomfort. Understanding how this progression happens can help you recognize when it’s time to seek care.
What Are Internal Hemorrhoids?
Internal hemorrhoids are swollen veins that develop inside the rectum. Because they are located internally, they often go unnoticed in the early stages.
Many patients first become aware of internal hemorrhoids when they experience symptoms such as:
- Painless rectal bleeding, often seen during bowel movements
- Mild discomfort or pressure
- A feeling of incomplete bowel emptying
At this stage, internal hemorrhoids are typically not visible and may not cause significant pain. However, that doesn’t mean they should be ignored.
Do internal hemorrhoids turn into prolapsed hemorrhoids?
Yes. Internal hemorrhoids can become prolapsed over time as the supporting tissues weaken and the swollen veins begin to protrude outside the anal opening, especially during bowel movements or straining.
How Internal Hemorrhoids Progress Over Time
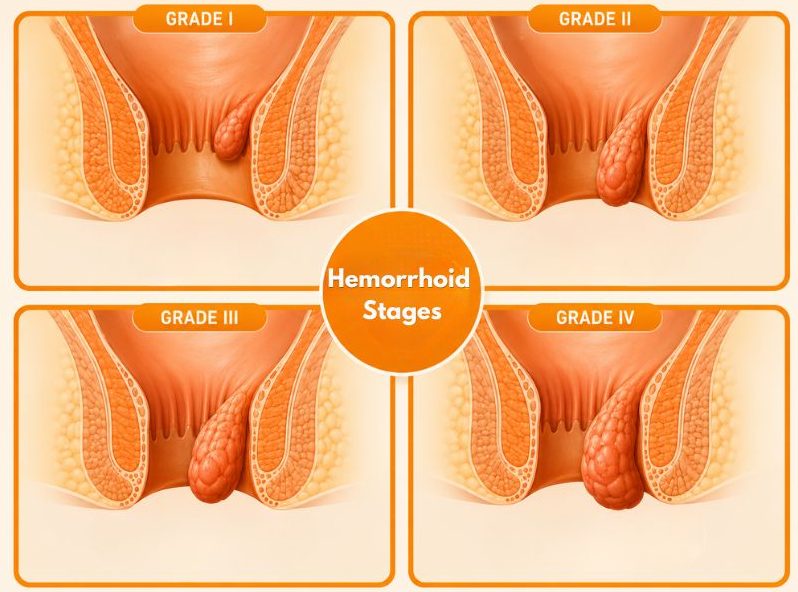
Internal hemorrhoids are classified into grades based on their severity. This grading system helps explain how they can evolve into prolapsed hemorrhoids:
- Grade I: Hemorrhoids remain inside the rectum and do not prolapse
- Grade II: Hemorrhoids may prolapse during bowel movements but return inside on their own
- Grade III: Hemorrhoids prolapse and must be manually pushed back inside
- Grade IV: Hemorrhoids remain prolapsed and cannot be pushed back in
As internal hemorrhoids advance from Grade I to Grade IV, the likelihood of prolapse increases. This progression often happens gradually, especially if underlying causes like straining, chronic constipation, or prolonged sitting are not addressed.
What is a Prolapsed Hemorrhoid?
A prolapsed hemorrhoid occurs when an internal hemorrhoid stretches and pushes outside the anal opening. This can lead to more noticeable and uncomfortable symptoms compared to earlier stages.
Patients with prolapsed hemorrhoids may experience:
- A visible lump or swelling outside the anus
- Increased discomfort or pain
- Irritation or itching
- Mucus discharge
- Difficulty keeping the area clean
In more advanced cases, prolapsed hemorrhoids can become trapped outside the body, which may lead to complications such as thrombosis (blood clot formation) or reduced blood flow.
Why Do Internal Hemorrhoids Become Prolapsed?
Several factors contribute to the progression from internal to prolapsed hemorrhoids. These include increased pressure in the lower rectum, which weakens the supporting tissues over time.
Common contributing factors include:
- Chronic constipation or straining during bowel movements
- Sitting for long periods, especially on the toilet
- Low-fiber diet
- Pregnancy
- Aging and weakening of connective tissue
When these pressures persist, the veins and surrounding tissues lose their ability to stay in place, eventually leading to prolapse.
When Should You Seek Treatment?
It can be tempting to ignore early symptoms, especially if they seem mild. However, early-stage internal hemorrhoids are often easier to treat and manage.
You should consider seeing a specialist if you notice:
- Recurrent rectal bleeding
- Persistent discomfort or pressure
- Any tissue protruding during or after bowel movements
- Symptoms that are worsening over time
Prompt evaluation not only confirms the diagnosis but also helps rule out other conditions with similar symptoms.
See Our Hemorrhoid Treatment Locations
Treatment Options for Internal and Prolapsed Hemorrhoids
Treatment depends on the severity of the hemorrhoids and your symptoms. Early-stage internal hemorrhoids may respond to lifestyle changes, such as increasing fiber intake and improving bowel habits.
However, as hemorrhoids progress, minimally invasive treatments may be recommended.
One advanced, non-surgical option is Hemorrhoid Artery Embolization (HAE). This outpatient procedure targets the blood vessels supplying the hemorrhoids. Using image guidance, a specialist reduces blood flow to the affected veins, which helps shrink the hemorrhoids and relieve symptoms over time.
Because HAE does not involve incisions or tissue removal, it offers a treatment option for patients seeking relief without traditional surgery.
The Importance of Early Diagnosis and Treatment
Internal hemorrhoids can absolutely progress into prolapsed hemorrhoids—but that progression is not inevitable. Early diagnosis plays a critical role in preventing symptoms from worsening and avoiding more advanced stages.
By addressing internal hemorrhoids early, patients may:
- Reduce the risk of prolapse
- Avoid increased discomfort and complications
- Access simpler, less invasive treatment options
How USA Hemorrhoid Centers Can Help
At USA Hemorrhoid Centers, our specialists focus on identifying hemorrhoids at their source and creating individualized treatment plans based on each patient’s needs. With advanced diagnostic tools and minimally invasive options like Hemorrhoid Artery Embolization, we help patients find relief before symptoms progress.
If you’re experiencing signs of internal hemorrhoids, getting evaluated sooner rather than later can make a meaningful difference in your comfort, your treatment options, and your long-term outcomes.
