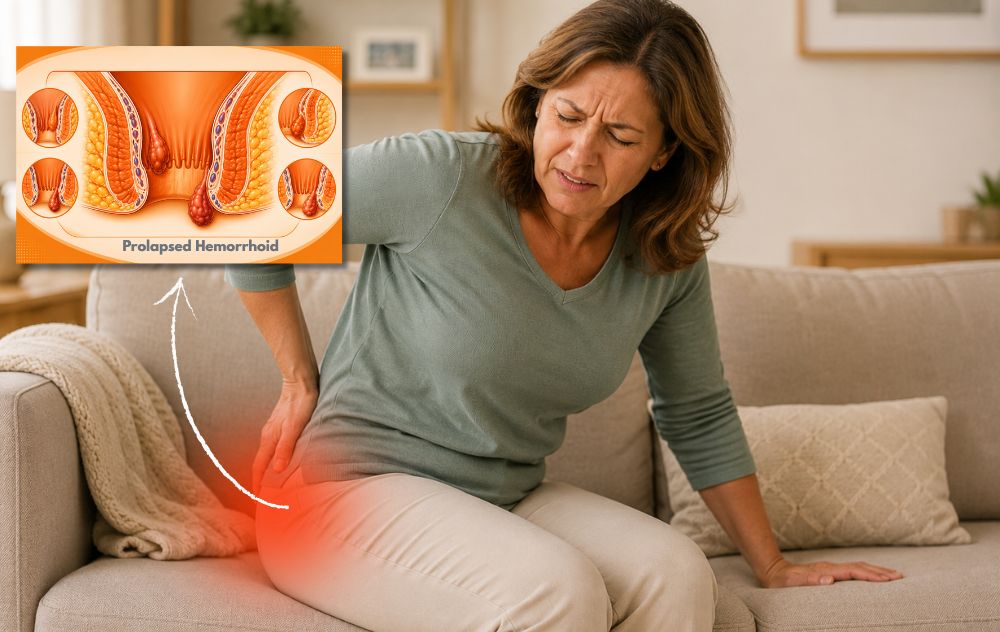
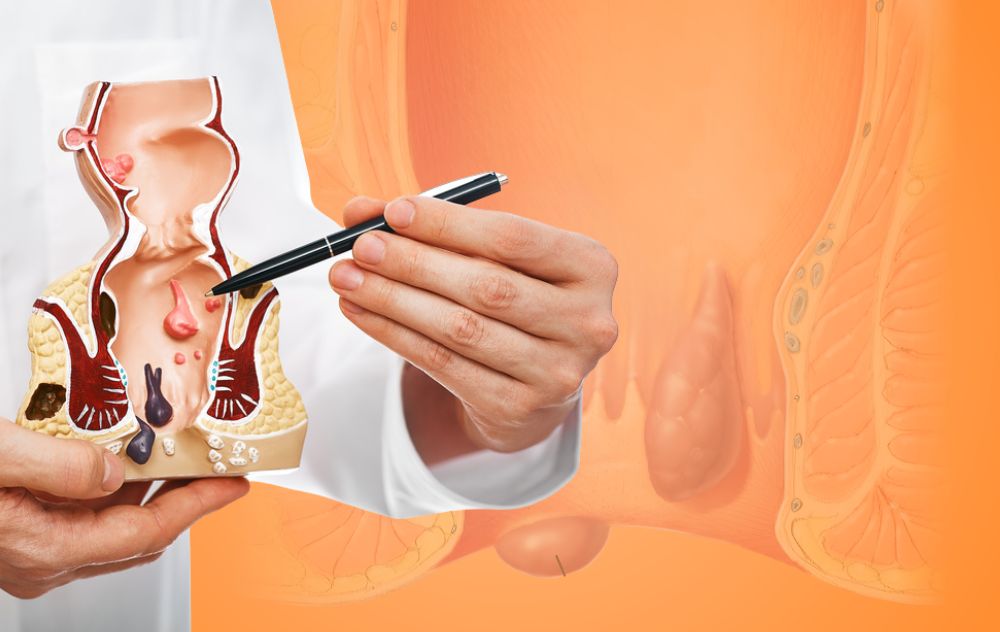
If you’re dealing with hemorrhoids, you’re not alone — and you’re probably not comfortable talking about it. Hemorrhoids are one of the most common digestive health conditions in the United States, affecting nearly 3 out of 4 adults at some point in their lives. They can cause pain, itching, swelling, and rectal bleeding — symptoms that can disrupt your daily routine and make even simple tasks uncomfortable.
The good news is that hemorrhoids are very treatable. But many people unknowingly make everyday choices — in how they eat, how they care for themselves, and how long they wait to seek help — that delay healing or make symptoms significantly worse. Knowing what not to do with hemorrhoids is just as important as knowing what helps.
This guide covers the most common hemorrhoid mistakes and what you should do instead.
1. Ignoring Symptoms and Delaying Treatment
One of the most damaging hemorrhoid mistakes is simply waiting and hoping things improve on their own. While mild hemorrhoids can sometimes resolve with rest and dietary adjustments, ignoring persistent symptoms allows the condition to advance — and more advanced hemorrhoids are significantly harder to treat.
Hemorrhoids that go unaddressed can:
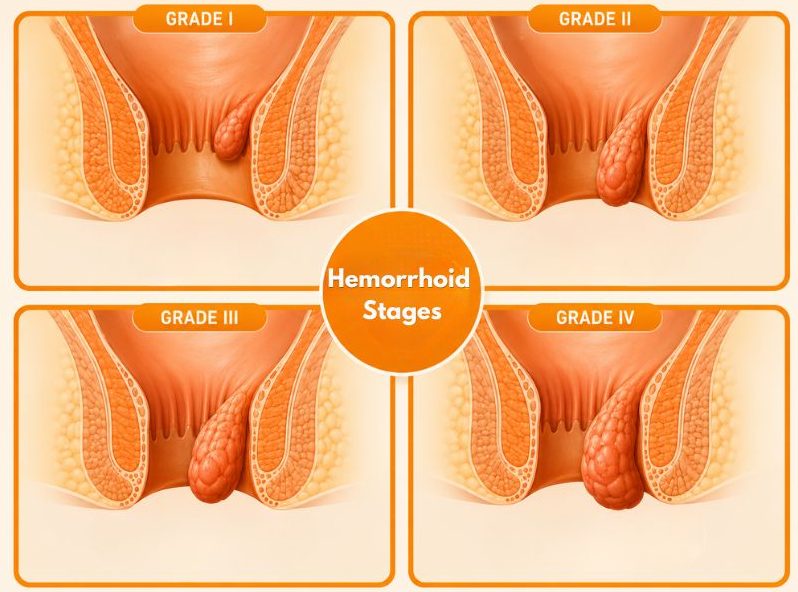
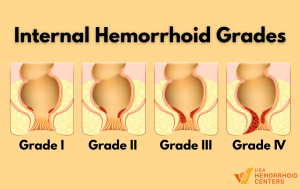
- Progress from Grade I (small, internal) to Grade III or IV (prolapsed, requiring intervention)
- Develop complications including thrombosis (blood clots) or tissue strangulation
- Cause chronic bleeding that increases the risk of anemia over time
Rectal bleeding in particular should never be self-managed without a professional evaluation. While hemorrhoids are a common cause, bleeding can also signal other conditions that require prompt diagnosis. Learn more about what happens when hemorrhoids are left untreated.
What to do instead: If symptoms last longer than one week, worsen, or include any rectal bleeding, contact a hemorrhoid specialist for an evaluation.
2. Straining During Bowel Movements
Straining is one of the primary drivers of hemorrhoid flare-ups — and one of the worst things you can do when hemorrhoids are already present. Bearing down on the toilet increases pressure in the rectal veins, causing hemorrhoids to swell further, bleed more, or prolapse.
Straining typically results from:
- Constipation caused by low fiber intake or dehydration
- Ignoring the urge to go and then forcing a bowel movement later
- Spending too long on the toilet, which increases rectal pressure even without active straining
What to do instead: Only go when you feel a natural urge. Never force a bowel movement. If constipation is a recurring problem, speak with your doctor about dietary fiber or stool softeners.
3. Poor Diet and Not Drinking Enough Water
What you eat directly affects your stool consistency — and stool consistency directly affects your hemorrhoids. A diet low in fiber produces harder, more difficult stools that require straining to pass. Over time, this repeated pressure is one of the most common causes of worsening hemorrhoid symptoms.
Common dietary mistakes that aggravate hemorrhoids include:
- Relying on processed foods, fast food, and refined grains (white bread, white rice, pasta)
- Not consuming enough fruits, vegetables, legumes, or whole grains
- Drinking alcohol or excess caffeine, which can dehydrate the body and harden stool
- Not drinking enough water throughout the day
What to do instead: Work toward approximately 14 grams of fiber for every 1,000 calories in your daily diet — ideally from whole food sources rather than supplements alone. Staying well-hydrated is equally important; aim for at least 6–8 glasses of water per day. For a detailed breakdown of what to avoid, see our guide on what foods trigger hemorrhoids.
4. Sitting for Long Periods — Including on the Toilet
Extended sitting puts sustained downward pressure on the veins in the rectal area, which can cause hemorrhoids to swell and worsen over time. This applies to desk work, long drives, and sedentary daily routines — but the toilet is often the most overlooked culprit.
Even sitting on the toilet for just 5–10 extra minutes per visit — whether due to phone use, reading, or waiting — increases rectal vein pressure significantly. The toilet opening acts like a mild vacuum on rectal tissue, and the longer you sit, the greater the effect.
What to do instead: Keep toilet visits brief and purposeful. At work, take short standing breaks every 30–60 minutes. If prolonged sitting is unavoidable, a donut-style cushion can help reduce direct pressure on hemorrhoidal tissue.
For guidance specifically on physical activities, exercises, and movements that affect hemorrhoids, see our detailed post on activities to avoid with hemorrhoids.
5. Using Harsh Soaps, Scented Wipes, or Irritating Products
Many people try to manage itching or discomfort by cleaning more thoroughly — but the wrong products can make hemorrhoid symptoms considerably worse. Scented, antibacterial, or alcohol-based cleansing products irritate already-inflamed tissue and can slow the healing process.
Products commonly associated with worsening hemorrhoid irritation include:
- Scented or alcohol-based wet wipes
- Antibacterial soaps with harsh surfactants
- Heavily fragranced toilet paper
- Over-the-counter hemorrhoid creams used more frequently or longer than directed
Aggressive or repeated wiping — even with soft tissue — can cause micro-tears that worsen inflammation and delay healing.
What to do instead: Clean the area gently with plain warm water after each bowel movement. Pat dry rather than rubbing. If itching continues, speak with your doctor before adding any new products to your routine.
6. Self-Diagnosing Without a Medical Evaluation
It is very common to assume that rectal discomfort, itching, or bleeding must be hemorrhoids. In many cases that assumption is correct — but several other conditions produce nearly identical symptoms, and missing them can have serious consequences.
Conditions that can mimic hemorrhoid symptoms include:
- Anal fissures — small tears in the anal lining causing sharp pain and bleeding
- Anal fistulas — abnormal tunnels near the anus that often require surgical correction
- Colorectal polyps or colorectal cancer — which can cause rectal bleeding, especially in adults over 45
- Inflammatory bowel disease (IBD) — including Crohn’s disease and ulcerative colitis
Treating the wrong condition with home remedies — or simply waiting — can allow a more serious condition to go undetected and untreated. To understand what symptoms should prompt an immediate evaluation, review our post on hemorrhoid warning signs and when to seek medical attention.
What to do instead: Get a professional diagnosis before beginning any treatment. A hemorrhoid specialist can evaluate your symptoms, rule out other conditions, and recommend the right approach for your specific situation.
7. Relying on Unproven Home Remedies
Not all home remedies are equal — and some popular ones can actively make hemorrhoids worse. A few to approach with caution:
- Apple cider vinegar applied directly: Undiluted vinegar applied to rectal tissue can cause chemical burns and significantly worsen irritation, despite being widely recommended online.
- Undiluted essential oils: Concentrated oils can cause contact dermatitis and allergic reactions in sensitive tissue.
- Ice applied directly to skin: While brief cold application can temporarily reduce swelling, direct skin contact with ice can cause tissue damage. Always use a cloth barrier and limit application time.
- Long-term OTC steroid cream use: Hydrocortisone-based products are appropriate for short-term use only. Prolonged application to rectal tissue can cause skin thinning. Use only as directed by a physician.
What to do instead: Warm sitz baths — soaking in a few inches of warm water for 10–15 minutes, two to three times per day — are among the most evidence-supported home measures for hemorrhoid discomfort. That said, no home remedy substitutes for professional evaluation when symptoms are persistent or worsening.
8. When to Stop Managing at Home and See a Specialist
Home care has a role in managing mild hemorrhoid symptoms — but there is a point at which self-treatment is no longer appropriate and professional evaluation becomes necessary. Do not delay seeking care if you experience:
- Any rectal bleeding — bright red blood on toilet paper or in the bowl
- Severe or sudden pain — particularly if accompanied by significant swelling
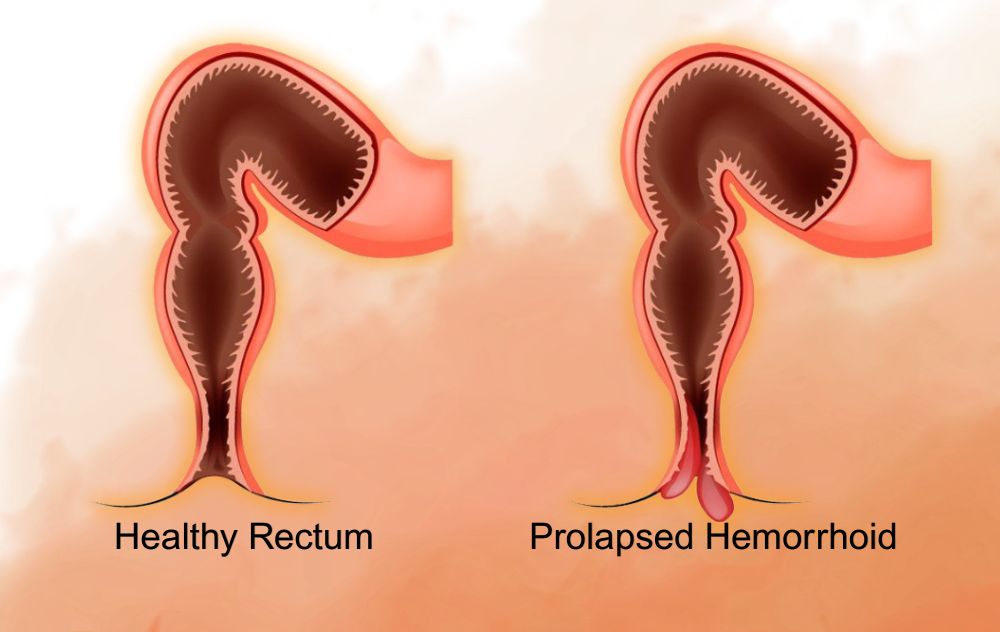
- A hemorrhoid that prolapses and will not return on its own
- Symptoms lasting more than 7–10 days despite consistent home care
- Recurring flare-ups that are becoming more frequent or more severe
- Any difficulty controlling bowel movements
Today, hemorrhoid treatment does not require surgery in most cases. Minimally invasive, in-office options — including rubber band ligation, sclerotherapy, infrared coagulation, and Hemorrhoid Artery Embolization (HAE) — are safe, effective, and designed to get you back to your routine quickly. HAE is a non-surgical procedure that reduces blood flow to the affected hemorrhoidal tissue, causing it to shrink naturally over time — with no general anesthesia, no hospital stay, and minimal recovery time.
A specialist can evaluate your symptoms and determine which treatment approach is the right fit for your condition and severity.
Conclusion: Stop Guessing — Start Healing
Hemorrhoid symptoms are uncomfortable, often embarrassing, and easy to mismanage. Whether it’s waiting too long to seek care, using the wrong products, eating a diet that worsens symptoms, or relying on unproven remedies — these common mistakes can turn a manageable condition into a more difficult one.
The most important step you can take is getting an accurate diagnosis from a qualified specialist. From there, a clear treatment plan — whether lifestyle-based or procedural — puts you in control of your symptoms rather than the other way around.
At USA Hemorrhoid Centers, our team of board-certified interventional radiologists provides compassionate, confidential hemorrhoid care using the most advanced evidence-based treatments available, including HAE. We have locations nationwide, accept most insurance plans including Medicare and Medicaid, and offer online scheduling with real-time insurance verification.
Frequently Asked Questions About Hemorrhoid Mistakes
When you have hemorrhoids, avoid straining during bowel movements, sitting on the toilet for extended periods, eating a low-fiber diet, and using harsh or scented personal care products near the affected area. You should also avoid self-diagnosing or delaying medical evaluation if symptoms are persistent, worsening, or include rectal bleeding.
Yes. Hemorrhoids that are not treated or managed appropriately can progress in severity. Internal hemorrhoids can advance from Grade I (small, internal only) to Grade III or IV (prolapsed and requiring manual replacement or surgical intervention). Thrombosed external hemorrhoids — where a blood clot forms — can cause significant pain and may require prompt medical treatment.
Foods that are low in fiber, highly processed, or dehydrating can make hemorrhoid symptoms worse by contributing to constipation and straining. This includes white bread, red meat, fast food, alcohol, and caffeinated beverages consumed in excess. Spicy foods may also irritate the digestive tract in some individuals. Focus on increasing dietary fiber and fluid intake to support regular, comfortable bowel movements.
You should see a hemorrhoid specialist if your symptoms have lasted more than one week, if you experience rectal bleeding of any amount, if a hemorrhoid has prolapsed and is not going back in on its own, or if your symptoms are significantly affecting your daily life. Early evaluation leads to more treatment options and faster relief.
Hemorrhoids themselves are not typically dangerous, but they should not be ignored — especially when rectal bleeding is involved. Rectal bleeding can occasionally signal more serious conditions, including colorectal cancer, which is why a professional evaluation is always recommended rather than assuming all symptoms are hemorrhoid-related.