A hemorrhoid bursting isn’t like popping a pimple. It’s not something you should try to make happen, nor is it a way to make a hemorrhoid go away safely. The experience of a burst hemorrhoid can be very alarming because of the blood loss. There’s also a risk of developing an infection in the area after the hemorrhoid bursts.
Let’s explore what causes a hemorrhoid to burst, the symptoms of a burst hemorrhoid, and when medical attention is necessary.
What Does It Mean for a Hemorrhoid to Burst?
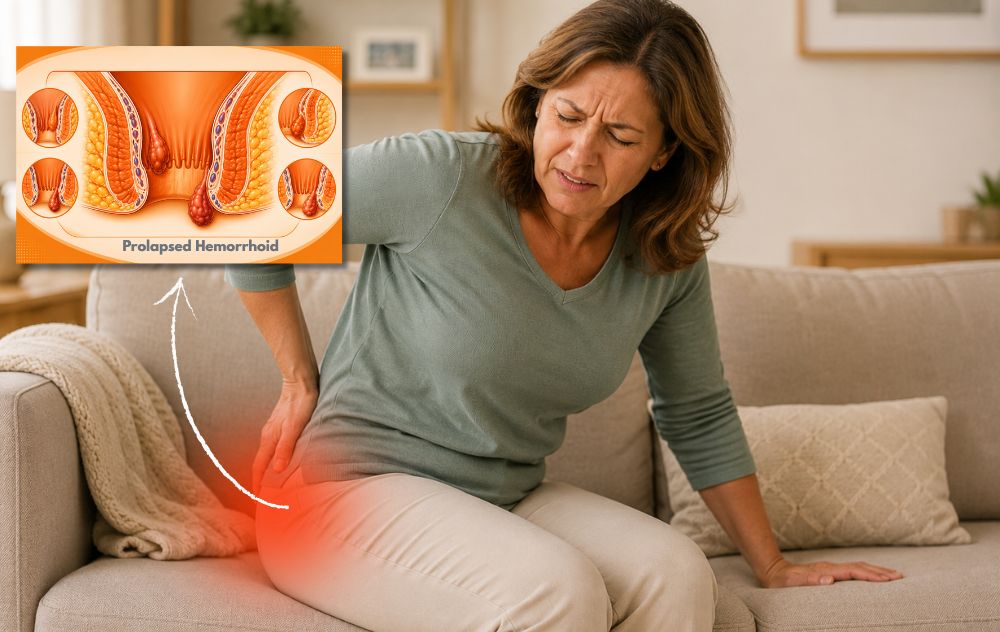
To understand a burst hemorrhoid, it helps to know that a hemorrhoid is essentially an enlarged, swollen vein located in or around the anus. A thrombosed hemorrhoid occurs when a blood clot forms inside one of these swollen veins. This clot causes the hemorrhoid to become very painful, firm, and often discolored.
A burst hemorrhoid happens when this thrombosed hemorrhoid, under significant pressure from the blood clot and associated swelling, tears through the surrounding skin. This leads to a sudden and often forceful release of blood, as well as other fluids or tissue.
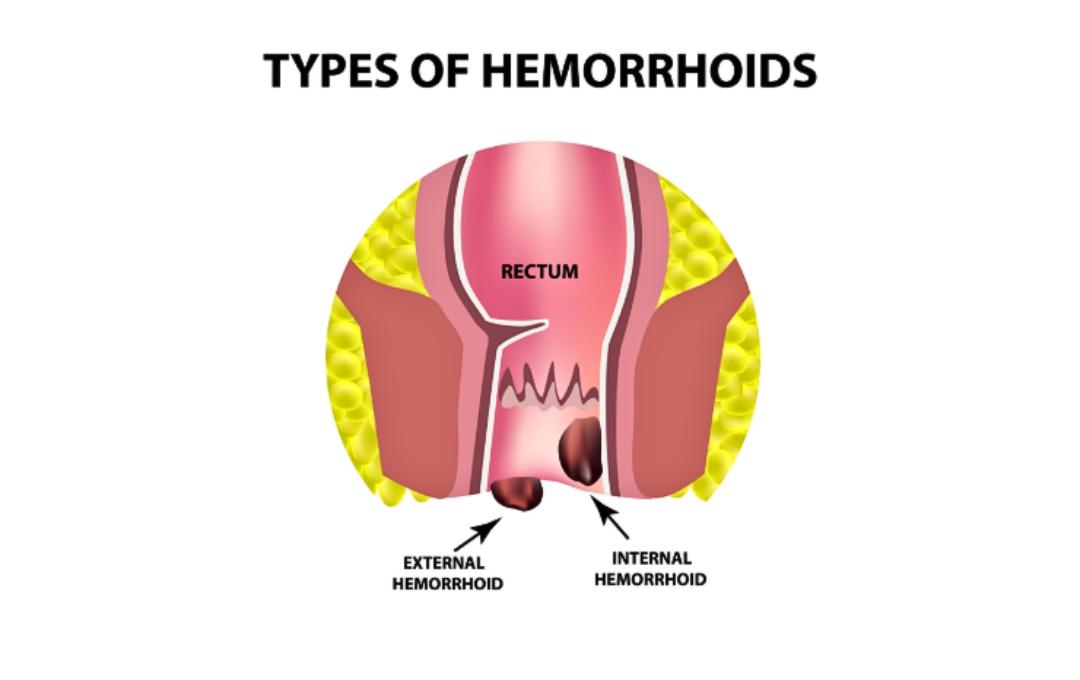
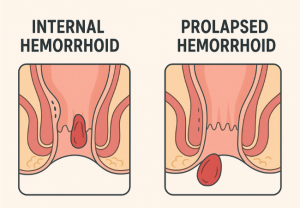
Hemorrhoids can form internally or externally. While external hemorrhoids are more likely to burst, both internal and external hemorrhoids can become thrombosed and rupture. Each type presents with different symptoms and may require different treatments.
- Internal hemorrhoids aren’t normally visible outside of the body, however, they can prolapse (slip out of its normal position) or protrude outside of the anus as a soft lump. Internal hemorrhoids rarely rupture, but they can if there’s enough pressure and the hemorrhoid has become prolapsed.
- External hemorrhoids are hard lumps that form under the skin, and they usually don’t require medical treatment.
Internal vs External Hemorrhoids Explained
Signs and Symptoms of a Burst Hemorrhoid
While a burst hemorrhoid generally presents with noticeable symptoms, the specific signs can vary depending on whether it’s an internal or external hemorrhoid that has ruptured.
Burst Internal Hemorrhoid
Internal hemorrhoids can cause minor bleeding. You might see a small amount of bright red blood in the toilet bowl or on toilet paper after a bowel movement. When an internal hemorrhoid bursts, the bleeding is sudden and usually happens all at once, and it can last for several minutes.
Signs and symptoms of a burst internal hemorrhoid include:
- Sudden release of bright red blood that can last for up to 10 minutes
- The release of a large blood clot
- Severe pain and discomfort in the affected area if the hemorrhoid is prolapsed
- Lightheadedness or dizziness from the blood loss
Usually, a burst internal hemorrhoid should be seen by a specialist. In some cases, a burst and bleeding hemorrhoid can be serious because of the risk of excessive blood loss, so it’s important to know when it’s a medical emergency.
Burst External Hemorrhoid
External hemorrhoids don’t normally cause bleeding. However, when they rupture, they can cause bleeding similar to what happens after an internal hemorrhoid bursts. Signs and symptoms of a burst external hemorrhoid include:
- Sudden, sharp pain
- Bright red or dark red blood on underwear, toilet paper, or in the toilet bowl
- Bleeding that may include a blood clot
- Tenderness when sitting
- Dizziness or lightheadedness
Can a Burst Hemorrhoid Kill You?
A burst internal or external hemorrhoid is likely not life-threatening. However, they can be dangerous if they cause an infection or if bleeding persists. Seek medical care if you notice any of the following issues along with a burst internal or external hemorrhoid:
- Continuous rectal bleeding
- Yellow discharge or pus leaking from the anus
- Severe pain
- A fever
To protect against serious complications, a doctor may recommend antibiotics for an infection. They can also help stop ongoing blood loss and rule out any other potential causes.
How Long Will a Burst Hemorrhoid Bleed?

A burst hemorrhoid will usually bleed for a few seconds or minutes. Bleeding from an internal hemorrhoid may be more long-lasting than bleeding from an external hemorrhoid. If the heavy bleeding continues for over ten minutes, you may need immediate medical care, as it may indicate a more serious issue.
There may also be some bleeding during bowel movements afterward, which will subside as the area heals. This can happen because a bowel movement can put pressure on the hemorrhoid, causing a short burst of bleeding.
Persistent anal bleeding caused by an internal hemorrhoid may require medical treatment.
What to Do When a Hemorrhoid Bursts
When a hemorrhoid bursts, apply a clean cloth to the affected area to help stop the bleeding. You can relieve discomfort and clean the area by taking a sitz bath, which is a warm, shallow bath. After a sitz bath, lightly dry the area with a clean towel. You can also use a cold pack to relieve swelling and pain.
After a hemorrhoid bursts, monitor the area for signs of an infection, such as an increase in pain or a yellowish discharge. The bleeding should also stop, although it’s not unusual to see bright red blood on the stool or toilet paper after bowel movements.
It’s recommended to see a hemorrhoid doctor if you have a ruptured internal hemorrhoid to help prevent complications and address any other existing internal hemorrhoids. If you’re unsure if a burst hemorrhoid is caused by an external hemorrhoid (which starts as a painful lump outside the anus) or an internal hemorrhoid (which is a soft lump that can protrude outside of the anus), a doctor can determine what type of hemorrhoid ruptured and how best to treat the area.
Can a Hemorrhoid Pop and Heal on Its Own?
A hemorrhoid that pops or bursts may heal on its own, although it can take a few weeks or longer to heal. However, just because a hemorrhoid has popped, it doesn’t mean that the hemorrhoid won’t develop symptoms again after it’s healed. Depending on a variety of risk factors, such as straining during bowel movements, hemorrhoids can start to bleed, itch, and swell due to more pressure on the rectal veins.
When to See a Doctor for Hemorrhoids
It’s important to see a doctor who treats hemorrhoids when symptoms persist after a week. The sooner persistent hemorrhoid symptoms are treated, the less likely the hemorrhoid is to burst.
Internal hemorrhoids often develop inside the rectum, so they may not cause noticeable discomfort right away. However, common internal hemorrhoid symptoms to look out for can include:

- Bright red blood on toilet paper or in the toilet after a bowel movement
- A feeling of fullness or pressure in the rectum
- Mucus discharge or a sensation of incomplete bowel emptying
- A prolapsed hemorrhoid that may temporarily push out of the anus
How to Treat Hemorrhoids Before They Burst
Internal hemorrhoids, including prolapsed and thrombosed hemorrhoids, can be treated with hemorrhoid artery embolization (HAE), a safe, effective alternative to hemorrhoid surgery. HAE is a non-surgical procedure that can be performed in an outpatient clinic, allowing patients to go home the same day as their treatment. It also has a short recovery and less risk of complications.
According to a 2024 study published in the World Journal of Gastroenterology, HAE has achieved a success rate of up to 93% in clinical studies and is well-known for offering long-lasting symptom relief.
LEARN MORE ABOUT HAE
About USA Hemorrhoid Centers
USA Hemorrhoid Centers is a national leader in providing specialized, non-surgical relief from hemorrhoids. We have a network of expertly trained doctors who specialize in treating internal hemorrhoids non-surgically with hemorrhoid artery embolization (HAE). We also treat hemorrhoid prolapse, thrombosed hemorrhoids, hemorrhoid bleeding, itching, and bowel discomfort.
Our clinics are accredited by the Accreditation Association for Ambulatory Health Care (AAAHC) because of our commitment to providing high-quality, patient-focused care. We accept most types of insurance and have affordable payment options available.
If you’re concerned about internal hemorrhoid symptoms, schedule a consultation at a USA Hemorrhoid Centers location near you. Treating internal hemorrhoids early on can help prevent a hemorrhoid from bursting. Our experienced doctors can also help prevent other problems caused by persistent hemorrhoids, including prolapse, severe pain, and infection.
SCHEDULE A CONSULTATION
FAQs About Burst Hemorrhoids
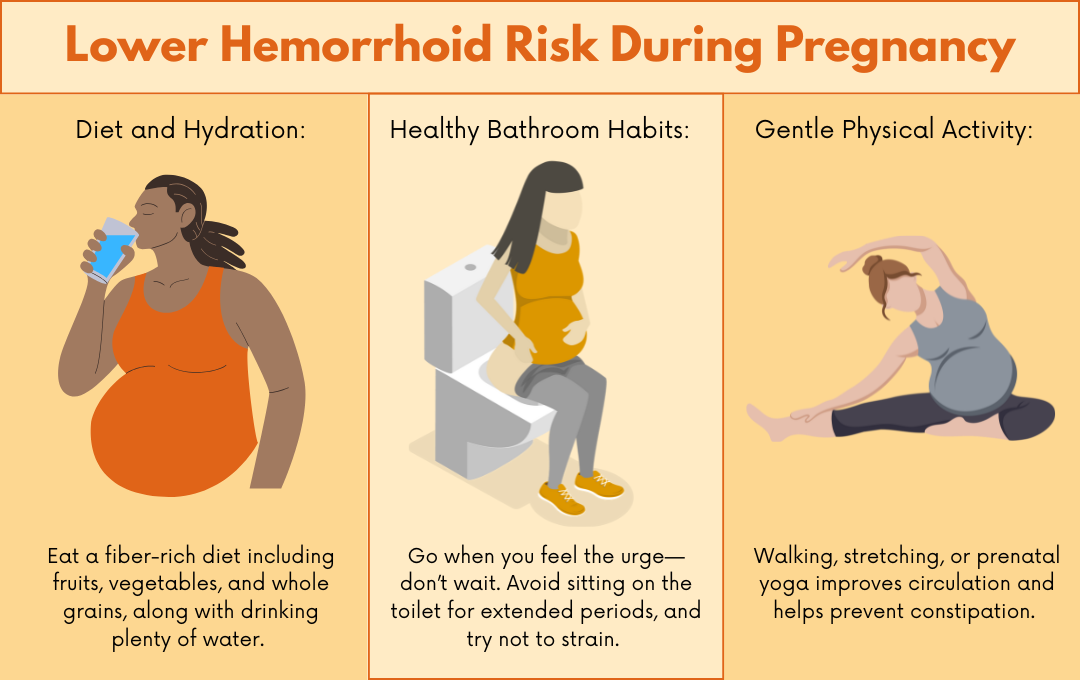
How can I prevent a hemorrhoid from bursting?
You can help prevent a hemorrhoid from bursting by avoiding straining during bowel movements and sitting for extended periods. These factors can irritate the hemorrhoid and make symptoms like swelling worse.
Can a hemorrhoid burst while sleeping?
A hemorrhoid can burst while sleeping if enough pressure builds up to cause the skin to break.
What helps a burst hemorrhoid heal faster?
Hemorrhoid treatment, like HAE, can help promote faster healing. Ice packs, sitz baths, and over-the-counter hemorrhoid ointments can also accelerate healing when used in conjunction with targeted medical treatment.