When you’re carrying extra weight, the physical strain on your rectal veins is relentless. You might have heard that losing weight is the ‘magic cure’ for hemorrhoids, but while dropping pounds, it doesn’t change the damage that’s already been done. These distended, swollen veins in the rectum and anus are incredibly common, but for those carrying extra body mass, the struggle is often more frequent and more severe.
The real trouble often starts where you can’t see it: internal hemorrhoids. These are the distended, swollen veins hidden inside the rectum that can bleed or prolapse without warning. For those carrying extra body mass, the weight acts like a constant, heavy hand pushing these internal veins out of place.
If you are struggling with flare-ups, you might be wondering: Can losing weight cure hemorrhoids? While weight loss significantly reduces pressure on your pelvic floor, once those internal veins have stretched and lost their elasticity, lasting relief usually requires a broader, comprehensive lifestyle and medical approach.
The Link Between Weight and Hemorrhoids
When discussing the connection between weight loss and hemorrhoids, it’s important to understand that your body’s circulatory system and your physical structure are deeply intertwined. Hemorrhoids are essentially varicose veins of the rectum; they occur when the veins in your lower gastrointestinal tract become swollen and inflamed.
While many factors contribute to this discomfort, excess body weight affects hemorrhoids in three primary ways:
- Vascular Strain (Intra-abdominal Pressure): Extra weight, especially around the midsection, pushes against rectal veins, causing them to stretch, lose elasticity, and distend into painful hemorrhoids.
- Gravity(Physical Load): Increased body mass intensifies the downward force on the pelvic floor. This constant gravitational stress, whether you are walking or sitting, weakens the tissues in the anus and rectum, making them more prone to bulging.
- Circulation Issues (Sluggish Blood Flow): Excess weight can act as a roadblock for blood returning to the heart. When blood “pools” or flows slowly through the lower body, rectal veins become engorged and inflamed, leading to chronic flare-ups.
Since poor circulation and vascular inflammation go hand-in-hand, achieving a healthier weight can be a helpful strategy for reducing the frequency and severity of flare-ups.
The Impact of Body Mass on Hemorrhoids
Even though diet is often the primary focus of the conversation, it isn’t the only link between your weight and rectal health. Beyond what you eat, the physical impact of carrying extra body mass creates a structural strain that directly promotes venous inflammation and swelling.
- Intra-Abdominal Pressure: The Constant Compression: Body weight concentrated in the midsection acts as a persistent internal weight. This intra-abdominal pressure compresses the pelvic floor, forcing the rectal veins to swell and distend. Even with a perfect diet, this physical pressure can keep veins engorged, making them more susceptible to injury and inflammation during daily activities.
- The “Structural” Shift: Extra weight can subtly alter the anatomical alignment of the rectum and pelvic floor. This shift makes the mechanics of a bowel movement more physically taxing. Because the angle of the exit is slightly compromised, the rectal veins endure higher levels of friction and strain, even when you aren’t straining manually.
The 4 Stages of Hemorrhoidal Internal Prolapse
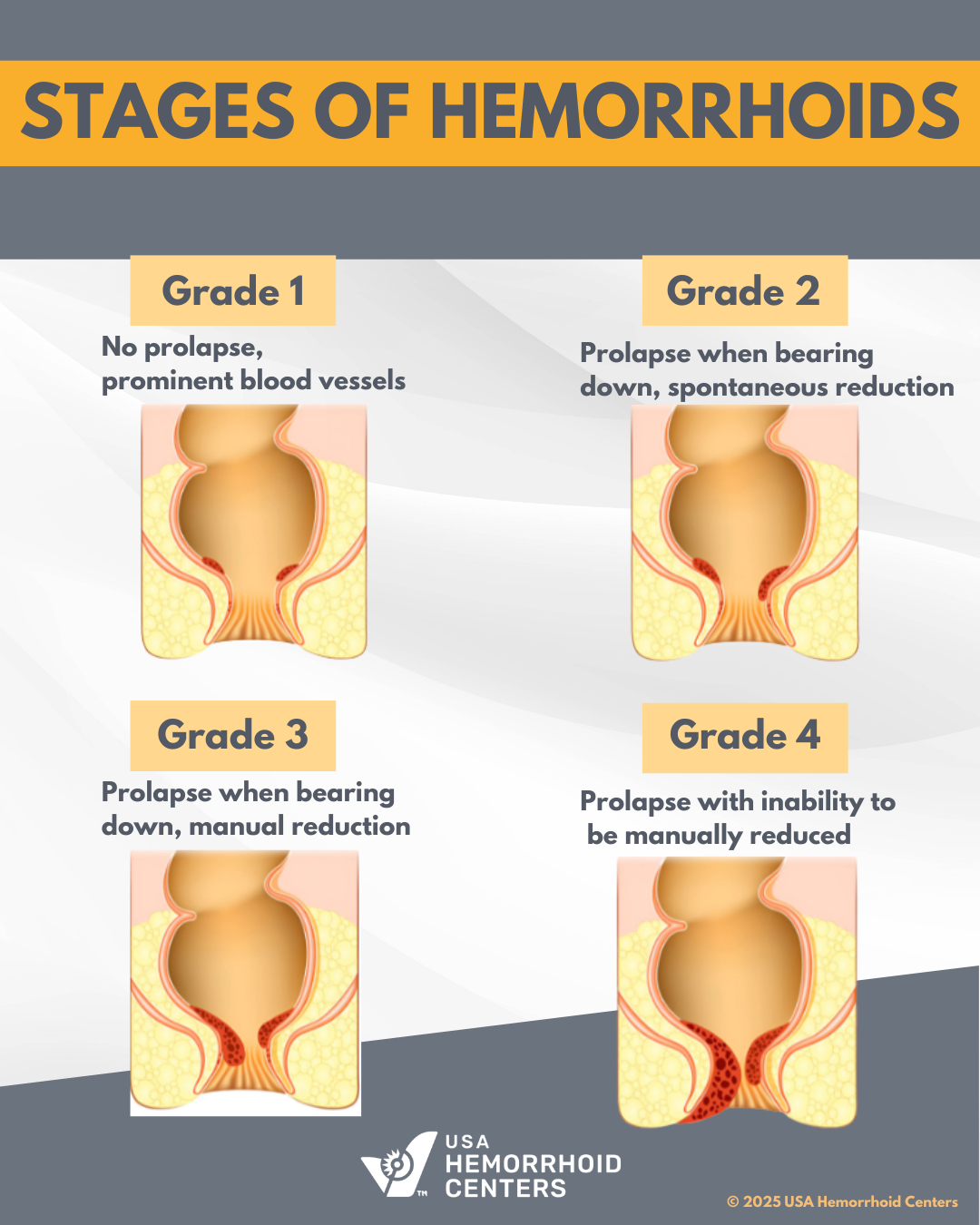
Medical professionals use a specific grading system to determine how far the hemorrhoidal tissue has moved from its original position.
The 1–4 Grading System
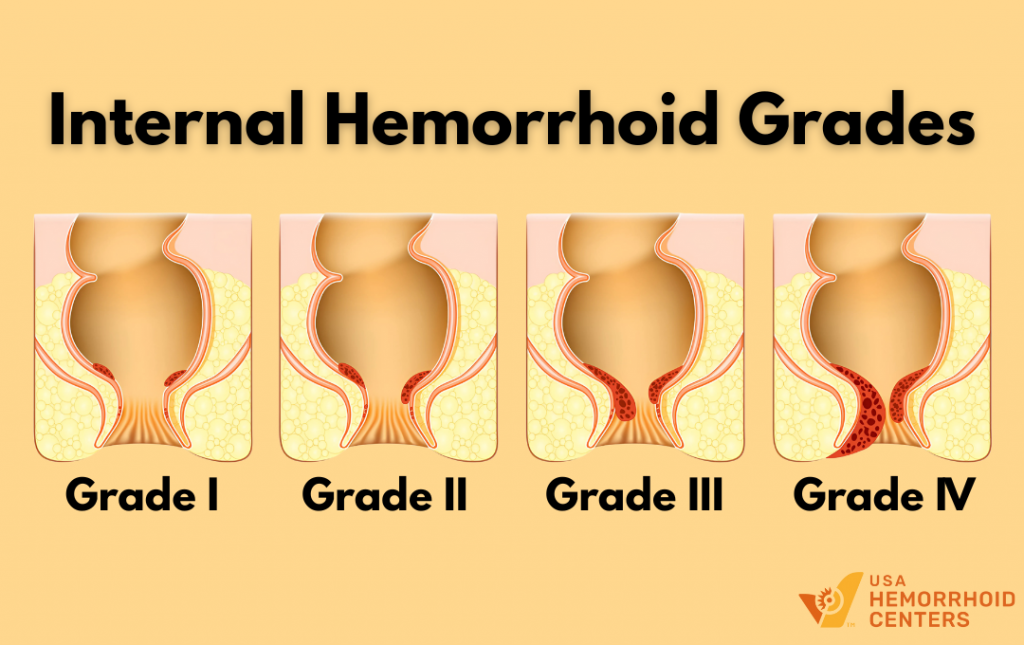
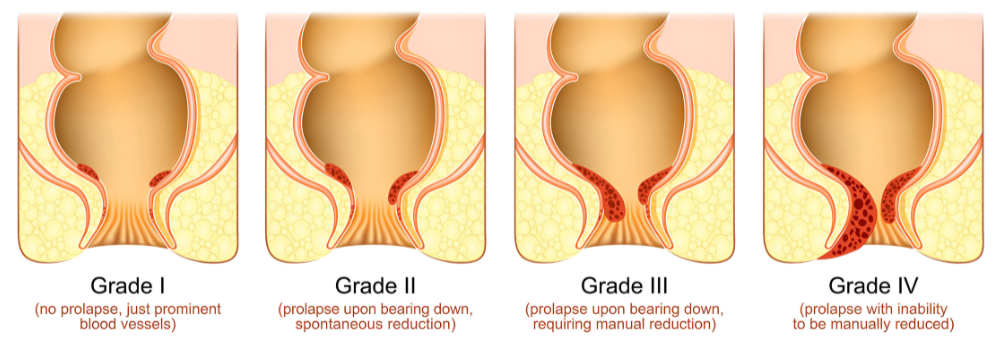
- Grade I: Internal hemorrhoids that bleed but do not prolapse (bulge out) of the anal canal.
- Grade II: Hemorrhoids that prolapse during a bowel movement but retract on their own.
- Grade III: Hemorrhoids that prolapse and must be manually pushed back inside.
- Grade IV: Permanent prolapse; the tissue remains outside the body and cannot be pushed back in.
Common Red Flags
Regardless of the grade, it is also important to keep an eye out for these primary symptoms:
- Pain, itching, and swelling: Often the first signs of localized inflammation.
- Bleeding: Noticing bright red blood during or after bowel movements.
- Prolapse: The sensation of tissue bulging or “dropping” outside the body.
- Fecal Leakage: In severe cases (Grade IV), the prolapsed tissue prevents the sphincter from closing fully.
Why Grading Matters for Weight-Related Hemorrhoids
For patients with a higher body mass, the progression through these stages can be significantly accelerated. The constant intra-abdominal pressure acts like a weight pushing the tissue downward 24/7. This means a Grade I issue can shift toward a Grade III much faster than in a lower-weight individual, as the pelvic floor is under continuous structural duress.
Learn More About Hemorrhoid Grades
How to Prevent Hemorrhoids with Weight Loss
Managing your weight is one of the most proactive steps you can take to alleviate the physical causes of rectal discomfort. When it comes to weight loss and hemorrhoids, the benefits are immediate and cumulative, focusing on reducing physical stress and improving internal health.
The BMI Connection
Clinical data suggests that the risk of developing chronic internal hemorrhoids increases significantly once a patient reaches a Body Mass Index (BMI) of 25 or higher. Entering the “overweight” or “obese” categories typically correlates with a measurable rise in intra-abdominal pressure. However, you don’t need to reach a “perfect” BMI to see results.
Reducing the Load: Lowering Pelvic Pressure
You don’t need to reach a perfect weight to see results. Research shows that even losing a small percentage of body weight, as little as 5% to 10%, significantly drops the intra-abdominal pressure on your pelvic veins.
By lightening the load, you reduce the mechanical strain that forces rectal veins to distend. Think of it as taking the weight off a literal spring; once the pressure is lifted, the veins have a much better chance of returning to their natural shape and staying there.
Improving Circulation: Boosting Vascular Health
Weight management does more than just lighten the physical load; it fundamentally improves the internal environment of your vascular system.
- Decreased Inflammation: Excess body fat can trigger systemic inflammation, which makes vein walls more brittle and prone to swelling. Weight loss helps cool this inflammatory response.
- Efficient Blood Return: As you lose weight, the demand on your cardiovascular system decreases. Improved circulation prevents blood from pooling in the rectal area, which is the primary cause of hemorrhoid bulging.
Why Weight Loss Alone May Not Be Enough
Even after significant weight loss, the vein walls in the rectum may remain stretched or weakened. Once an internal hemorrhoid has developed, it may require medical intervention to shrink the vessel and restore proper blood flow.
Taking the First Step Towards Relief
While weight loss is a powerful long-term strategy to reduce pressure and prevent future flare-ups, it isn’t always a “quick fix” for existing damage. Once rectal veins have significantly distended, the structural changes to the vein walls are often permanent. At this stage, lifestyle modifications should be viewed as a way to manage symptoms, while medical intervention is necessary to treat the source. Pairing a healthier BMI with minimally invasive treatments ensures that you are not only removing the external pressure but also repairing the internal damage for lasting relief.
Beyond Home Remedies: Addressing the Pain
Depending on the severity or grade of your condition, your treatment path will vary. Immediate pain management often requires a tiered approach:
- Self-Care (Grade 1): For mild swelling, conservative at-home methods can provide temporary relief. Sitz baths (soaking in warm water) help relax the anal sphincter, while over-the-counter topical treatments or wipes can reduce local inflammation.
- Medical Intervention (Grades 2 & 3): If hemorrhoids prolapse (protrude) during bowel movements, weight loss alone may not be enough to retract the damaged tissue. In these advanced stages, the physical structure of the vein has been compromised, requiring professional clinical treatment.
The Non-Surgical Solution: Hemorrhoid Artery Embolization (HAE)
For those dealing with obesity and hemorrhoids and seeking a permanent solution without the painful recovery of traditional surgery, hemorrhoid artery embolization (HAE) has emerged as a leading minimally invasive option.
Hemorrhoid Artery Embolization (HAE): How It Works
Unlike a hemorrhoidectomy, which involves cutting tissue, HAE addresses the problem at the source, the blood supply.
- A specialist inserts a tiny catheter (usually through a small nick in the wrist or groin).
- Using advanced imaging, they locate the specific branches of the superior rectal artery that feed the hemorrhoids.
- Small “coils” or particles are placed to reduce blood flow to those specific veins.
- Without the excess blood pressure, the hemorrhoids naturally shrink and disappear over time.
The Benefits of HAE
- No Cutting or Stitches: Because it is performed through the arteries, there is no trauma to the sensitive rectal tissue.
- Quick Recovery: Most patients return to normal activities within a day or two.
- High Success Rate: It effectively treats internal bleeding and discomfort with significantly less post-procedure pain than surgical alternatives.
When to See a Specialist
While lifestyle changes are vital, some situations require more than just home remedies or a change in diet. Recognizing when your condition has progressed beyond self-management is key to avoiding long-term complications. If you experience any of the following, it is time to consult a professional:
- Chronic Bleeding: Any rectal bleeding should be evaluated to rule out more serious conditions.
- Persistent Pain: Discomfort that disrupts your daily life or sleep.
- Stage 3 & 4 Protrusions: Hemorrhoids that prolapse (fall out) and either require manual reinsertion or cannot be pushed back in at all.
Find Relief with USA Hemorrhoid Centers

While focusing on weight loss and hemorrhoids helps reduce the “root cause” pressure, it may not be enough if the vascular damage is already done. Once veins have significantly distended, they often stay that way regardless of how much weight you lose. Waiting too long can allow the tissue to further weaken, making future treatments more complex.
At USA Hemorrhoid Centers, we recognize that even with successful weight loss, hemorrhoids caused by years of vascular strain may not simply disappear. If lifestyle changes haven’t provided the relief you need, we offer a long-term, minimally invasive solution: hemorrhoid artery embolization (HAE).
Our experienced physicians specialize in vascular health and are dedicated to helping you find a permanent solution to persistent hemorrhoid discomfort. HAE is often the ideal next step for patients who haven’t found lasting results through diet, exercise, or previous medical procedures like rubber band ligation. If your symptoms are flaring up and stalling your health journey, our expert team is ready to help. Schedule a consultation online today or call (855) 805-4247 to see if HAE is right for you.
FAQs
Will losing weight make hemorrhoids go away?
Weight loss can significantly reduce the pressure on your pelvic veins, which often shrinks existing hemorrhoids and prevents new ones from forming. However, if the veins are severely stretched (Stage 3 or 4), they may remain present even after weight loss, requiring medical intervention to resolve fully.
What is the best way to get rid of hemorrhoids?
The most effective approach is a combination of lifestyle prevention and clinical treatment. First, you must address the cause of the condition to reduce internal pelvic pressure. However, for persistent internal hemorrhoids, medical intervention such as Hemorrhoid Artery Embolization (HAE) is the most reliable solution. This non-surgical procedure provides long-term relief by targeting the blood supply at the source, allowing damaged veins to shrink without traditional surgery.