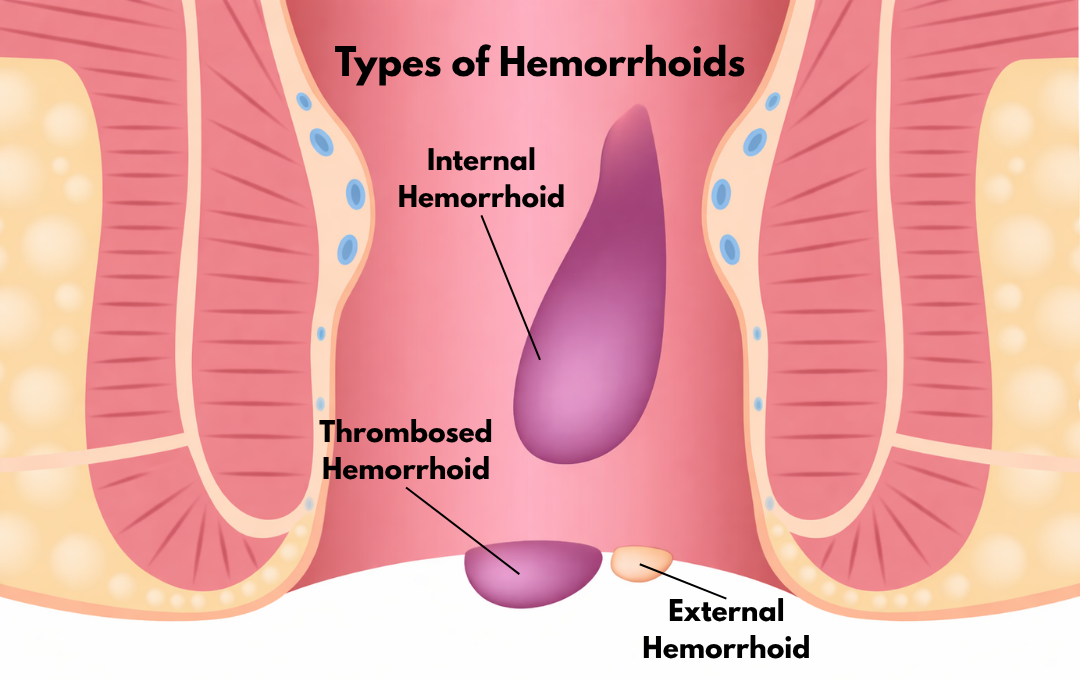
Childbirth often comes with physical surprises, including the discomfort of postpartum hemorrhoids. Internal hemorrhoids are swollen veins in the rectum or anus that affect about 25% to 40% of new mothers. Hemorrhoids appear in two forms: internal hemorrhoids, which are located inside the rectum and are usually painless despite potential bleeding, and external hemorrhoids, which develop around the anus and often cause itching or pain.
Whether triggered by the pressure of an enlarged uterus or the intense physical strain of delivery, hemorrhoids are very common parts of the body’s recovery process. This post explores why they occur and highlights modern, minimally invasive treatments to help you find relief comfortably.
Why Do Hemorrhoids Occur During Pregnancy and Childbirth?
The development of postpartum hemorrhoids is the result of an internal chain reaction. As the baby grows, the heavy uterus presses directly against the main pelvic and abdominal veins. This pressure acts like a roadblock, slowing down the flow of blood from your lower body back up to your heart. Because the blood cannot drain upward efficiently, it pools in the lowest branches of this vascular network—the veins in the rectum—causing them to stretch, swell, and become hemorrhoids.
Hormonal Shifts
During pregnancy, your body produces high levels of a hormone called progesterone. While progesterone is essential for supporting your pregnancy, it has a systemic muscle-relaxing effect that triggers hemorrhoids in two simultaneous ways:
- It relaxes your vein walls: Progesterone softens the muscular walls of your blood vessels. Because the veins are less firm, they stretch out, sag, and swell much more easily under the weight of your blood flow.
- It slows down your digestion: That same relaxing effect calms the muscles in your digestive tract. This slows your digestion to a crawl, causing constipation. Passing hard stools forces you to strain, putting massive extra pressure on those already softened rectal veins.
Physical Force of Labor
If hormones and a growing baby lay the groundwork, the intense pushing during labor and delivery is often the final physical trigger.
The extreme straining required to deliver a baby creates a sudden, massive surge of pressure right in your pelvic floor. This intense physical force acts like a pump, instantly forcing blood into the rectal veins, causing them to balloon, swell, or push completely outside the body.
Hemorrhoids After Cesarean Section
Worsening internal and external hemorrhoids after a cesarean section are also possible. While they are more common after vaginal births, the pressure on pelvic veins during pregnancy, postpartum hormonal constipation, and limited mobility after surgery contribute to their development. They usually appear within the first few weeks postpartum.
Postpartum hemorrhoids can complicate the healing process of C-sections by:
- Increasing overall pain, making it harder to move comfortably during surgical recovery.
- Causing straining from post-operative constipation (often triggered by pain meds), which puts unwanted pressure on the abdominal incision.
To support recovery, doctors usually recommend conservative care, such as high-fiber diets and stool softeners, to ensure bowel movements are easy and do not interfere with the healing of the surgical site.
Common Risk Factors
While any pregnancy can lead to hemorrhoids, certain factors increase the likelihood:
- Prolonged labor: Labor lasting 12+ hours or a prolonged second (pushing) stage.
- Gestational length: A pregnancy that extends past 40 weeks.
- Birth weight: Delivering a newborn with a heavy birth weight.
- Spontaneous childbirth: Rapid or unassisted delivery stages.
- Lifestyle factors: Chronic constipation caused by a slowed digestive tract or a sedentary lifestyle.
Seeking Relief: How to Treat Postpartum Hemorrhoids
One of the most common postpartum complications is a thrombosed external hemorrhoid, which occurs when a painful blood clot forms within a swollen vein just under the skin. To prevent complications like inflammation, prolapse, or further thrombosis, early treatment is key.
Most doctors recommend starting with conservative treatments, such as increasing fiber intake, staying hydrated, avoiding constipation, and practicing healthy bathroom habits. These simple adjustments are often enough to allow the body to heal naturally.
However, if symptoms persist after a month of conservative care, minimally invasive procedures, such as hemorrhoidal artery embolization (HAE), may be considered. More aggressive surgical options are rarely recommended while a woman is breastfeeding.
Symptoms to Watch For
Postpartum hemorrhoids can vary in sensation, but there are several common signs to keep on your radar. Many people notice lumps around the anus, ranging in size from a small pea to a grape. These are often accompanied by itching, burning, or general rectal discomfort that makes sitting or moving around feel uneasy.
You may also experience pain during or after bowel movements. If you notice bright red blood on the toilet tissue or in the bowl, it is typically a sign of a hemorrhoid being irritated. While these symptoms are common, keeping track of them can help you determine when it’s time to move from at-home care to a conversation with your healthcare provider.
How Long Do Hemorrhoids Last After Childbirth?

Right after childbirth, a woman’s hemorrhoids can appear “large and alarming,” but they typically begin to shrink within a few days. While hemorrhoids are usually at their most painful during the first five days, most people notice significant improvement by the two-week mark. This relief happens naturally as the uterus shrinks and blood volume decreases, reducing the overall pressure in the pelvic and anal area.
While the majority of postpartum hemorrhoids resolve on their own within six to 12 weeks, some may require medical attention. In some instances, you may notice small skin tags remaining after the swelling goes down; this occurs when the body reabsorbs the blood, but the stretched skin stays behind.
How to Tell the Difference: Hemorrhoids vs. Postpartum Bleeding
The easiest way to tell them apart is to look at the color of the blood, when it appears, and where it lands.
Postpartum Bleeding (Lochia)
Postpartum bleeding (Lochia) is the completely normal shedding of the uterine lining after giving birth.
- The Location: This blood comes directly from the vagina.
- The Appearance: In the first few days, it is dark red or deep crimson and flows like a heavy menstrual period, often containing small blood clots. Over a few weeks, it naturally changes color from red to pink, brown, and eventually a yellowish-white.
- The Timing: It is a continuous, steady flow that will be present on your maternity pad throughout the day, regardless of whether you are resting or using the bathroom.
Postpartum Hemorrhoid Bleeding
Hemorrhoid bleeding comes from stretched veins at the exit of the digestive tract.
- The Location: This blood comes strictly from the anus.
- The Appearance: This blood is bright, vivid red because it is fresh, oxygen-rich blood from a breached vein. It never looks brown or yellowish.
- The Timing: It is intermittent and almost always triggered by a bowel movement. You will typically only see it as a streak on your toilet paper, a splash in the toilet bowl after straining, or coating the surface of a hard stool. It does not pool continuously on a maternity pad while you are just resting.
Will Postpartum Hemorrhoids Go Away?
While postpartum hemorrhoids are common, certain symptoms require professional medical attention to ensure a smooth recovery. You should contact your healthcare provider if you experience:
- Heavy or persistent rectal bleeding.
- Severe pain that interferes with your daily activities or makes nursing uncomfortable.
- A hard, purple hemorrhoid can indicate the formation of a blood clot (thrombosis).
- Symptoms that show no improvement after a week of consistent home care.
Addressing these signs early can help prevent complications and ensure you get the most effective treatment for your specific needs.
Can Postpartum Hemorrhoids Return?
If you are planning another pregnancy, hemorrhoids may likely recur. Healthcare providers note that if they are present at the start of a subsequent pregnancy, they may worsen as the trimesters progress. However, the same recovery pattern typically applies, with the veins shrinking or resolving significantly once again after delivery.
At-Home Relief

If you are experiencing discomfort from postpartum hemorrhoids, several gentle, at-home strategies can provide significant relief and support the healing process.
- Hygiene Habits: Swap dry toilet paper for a bidet or witch hazel wipes. These options clean sensitive areas without the friction that can irritate swollen veins.
- Soothe the Swelling: Use temperature to your advantage. Alternating between ice packs to reduce inflammation and warm sitz baths to relax the muscles can help manage pain throughout the day.
- Over-the-Counter Help: For immediate relief, consider topical creams or stool softeners. These are excellent short-term tools to reduce itching and make bathroom trips more comfortable.
Preventive Postpartum Hemorrhoids Care
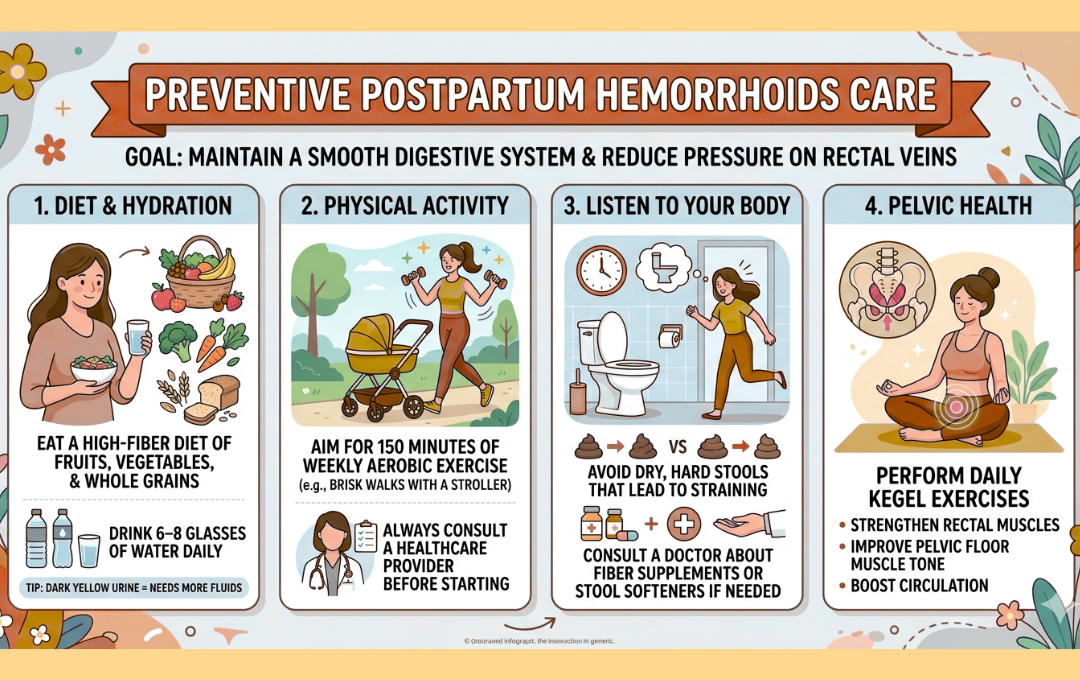
Preventing postpartum hemorrhoids is possible. The most effective strategy is to keep your digestive system moving smoothly to reduce pressure on your rectal veins.
- Focus on Fiber and Hydration: A high-fiber diet filled with fruits, vegetables, whole grains, and beans is your best defense. Pair this with plenty of water—aim for six to eight glasses a day. A quick tip: if your urine is dark yellow, it’s usually a sign you need to hydrate more.
- Stay Active: Aim for 150 minutes of aerobic exercise per week, which helps boost energy and keep your digestive tract moving. Even a short, brisk walk with the stroller counts! Just be sure to check with your healthcare provider before starting an exercise routine postpartum.
- Listen to Your Body: If you feel the urge to go, don’t wait. Delaying a bathroom break can make stool drier and harder to pass, leading to the straining that causes hemorrhoids. If you are struggling with constipation, ask your doctor if a fiber supplement or stool softener is right for you.
- The Power of Kegels: While often associated with bladder control, daily Kegel exercises also strengthen the muscles around the rectum. Improving muscle tone in the pelvic floor can help support your veins and improve overall circulation in the area.
Advanced Care: Hemorrhoid Artery Embolization (HAE)
While many postpartum hemorrhoid cases resolve with lifestyle changes, medical intervention becomes necessary when symptoms persist beyond a month or involve complications like thrombosis (clotting) or prolapse (veins protruding outside the body). If conservative methods like high-fiber diets and stool softeners haven’t provided relief, it may be time to discuss more advanced, minimally invasive options with a hemorrhoid specialist.
What is Hemorrhoid Artery Embolization (HAE)?
Hemorrhoid artery embolization (HAE) is a modern, non-surgical treatment designed to target the root cause of the discomfort. During this procedure, a specialist uses a thin catheter to reach the specific arteries supplying blood to the hemorrhoids. By placing tiny coils or particles to reduce this blood flow, the internal hemorrhoids naturally shrink and heal.
Because HAE is performed through a catheter, often in the wrist or groin, it typically involves less pain and a much faster recovery time than other hemorrhoid removal methods.
How HAE Works:
- Targeted Access: A specialist inserts a tiny catheter to reach the specific rectal arteries supplying the hemorrhoids.
- Embolization: Small particles called microspheres are released to block the specific blood vessels feeding the hemorrhoid.
- Natural Resolution: Deprived of its blood source, the hemorrhoid eventually shrinks and withers away, eliminating the need for invasive cutting or stitches.
Is Hemorrhoid Artery Embolization (HAE) Safe After Childbirth?
For those seeking relief, hemorrhoid artery embolization (HAE) is a modern, nonsurgical option that is considered very safe for postpartum patients. Unlike standard surgery, HAE involves no incisions or stitches in the rectal area, significantly reducing the risk of infection and shortening recovery time.
A primary benefit for postpartum mothers is that HAE does not typically require general anesthesia, making it a safer alternative for those managing the physical demands of a newborn. Furthermore, because it is a localized procedure that doesn’t rely on heavy medications, it is often a viable option for mothers who are breastfeeding.
More importantly, HAE does not interfere with the natural healing of the uterus after vaginal delivery or a C-section. Since the procedure specifically targets the blood flow to the rectal arteries rather than the uterine arteries, it allows the uterus to continue its recovery process undisturbed. This makes it an ideal solution for mothers who need to address hemorrhoid pain without complicating their overall postpartum healing.
Postpartum Hemorrhoid Care at USA Hemorrhoid Centers
If conservative treatments aren’t providing the relief you need, you don’t have to go through a long surgical recovery. At USA Hemorrhoid Centers, our highly skilled hemorrhoid specialists understand the unique physical challenges that postpartum mothers face. We offer hemorrhoidal artery embolization (HAE), an outpatient procedure with a significantly shorter recovery time than traditional surgery, so that new mothers can get back to their families quickly.