We’ve all done it — we’ve brought something into the bathroom to pass the time as we do our “business.” Back then, we skimmed magazines and browsed catalogs. Today, it’s scrolling through social media or reading an interesting article you found online.
Regardless of how we occupy our time in the bathroom, this seemingly harmless habit may contribute to an issue many are too embarrassed to talk about: hemorrhoids.
Spending too much time on the toilet can strain the blood vessels inside the rectum. While hemorrhoids usually help with bowel movements, too much pressure in the rectal veins can cause flare-ups with symptoms like bleeding, itching, pain, and swelling. Understanding the effects of “toilet scrolling” on hemorrhoids can help people find ways to prevent hemorrhoids or find effective treatment options that alleviate symptoms.
The Medical Link: Why Doctors Warn Against ‘Toilet Scrolling’
A cross-sectional study conducted at the Public Library of Science found a link between smartphone use on the toilet and hemorrhoid flare-ups.1 People who used their phones while on the toilet had a 46 percent higher prevalence of inflamed hemorrhoids compared to those who did not. This can happen for the following reasons:
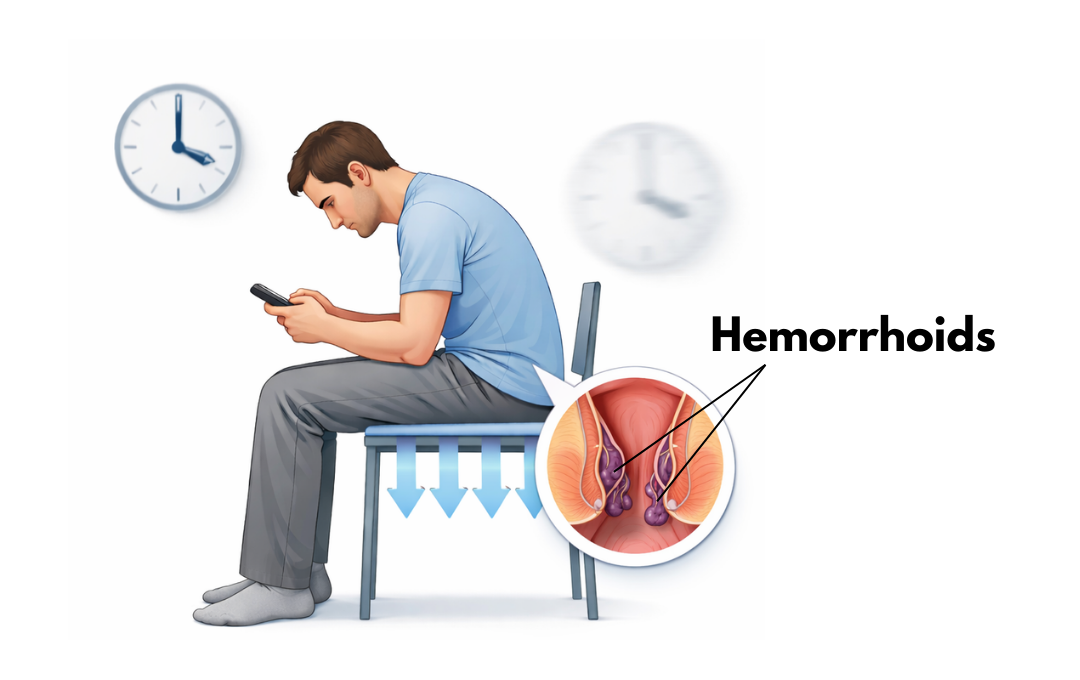
The “Sinkhole” Effect: Unlike chairs or sofas, toilet seats do not support the pelvic floor muscles that help keep the rectum in place. Without support, the pelvic floor muscle relaxes, and gravity adds pressure to the rectal veins. Over time, this pressure can cause hemorrhoids to swell and start to bleed.
The Time Factor: As authors of the study note, the high stimulation from smartphones can cause users, primarily men, to lose track of time when going to the bathroom. This can lead to more time spent sitting on the toilet that further adds to pressure on the rectal veins.
The Gravity Problem: How Prolonged Sitting Strains Your Veins
Prolonged sitting is not limited to the toilet. Whether you frequently travel, work a full day behind a desk, or relax for extended periods, sedentary habits can impact overall circulation.
Being in one position for hours can slow blood flow — especially in areas farthest from the heart, such as the legs and lower rectum. Over time, reduced blood flow can lead to vein-related issues, including varicose veins and hemorrhoid flare-ups.
While sitting alone does not cause hemorrhoids, prolonged sitting combined with straining during bowel movements, low-fiber diets, and dehydration can increase the risk of flare-ups.
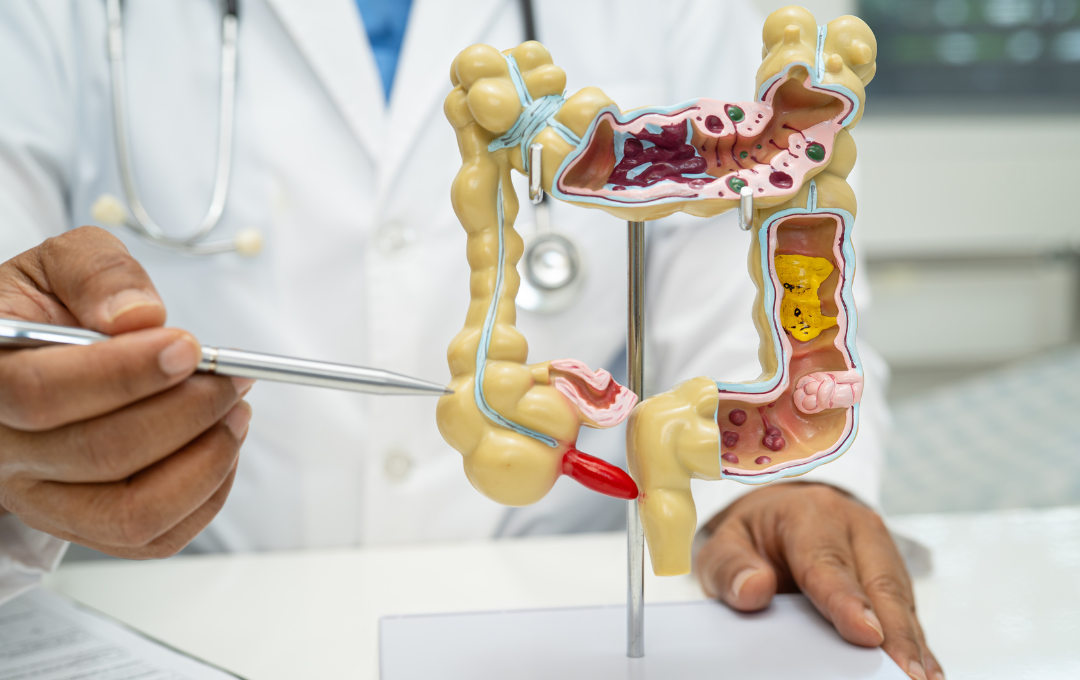
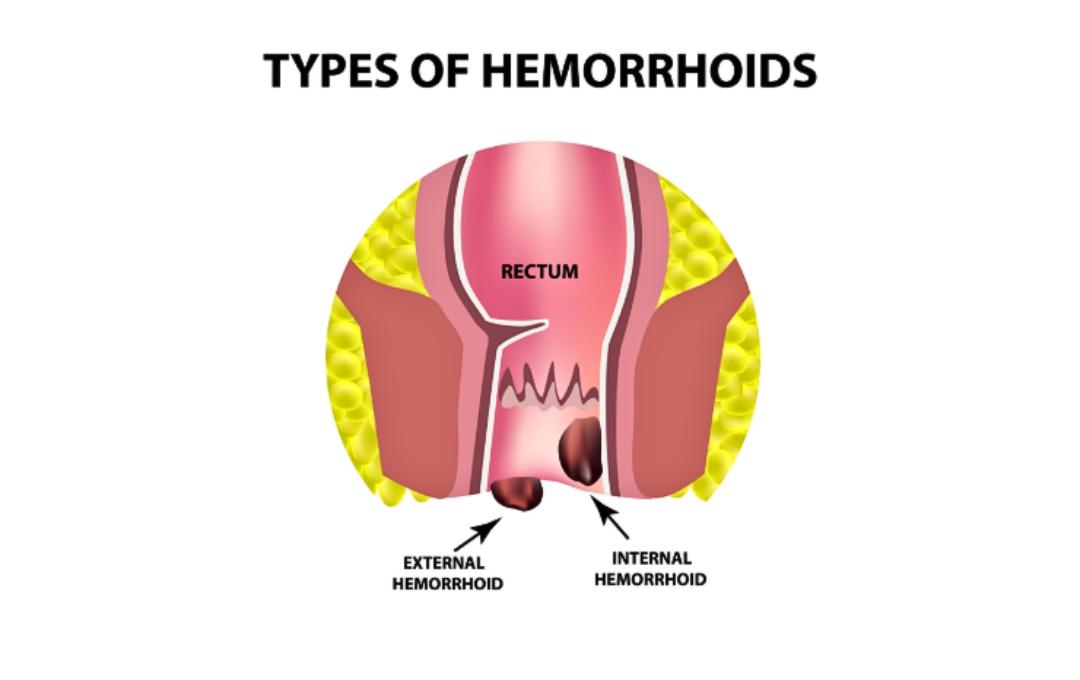
Internal vs. External Hemorrhoids: What’s the Difference?
Depending on the patient, the pressure from prolonged sitting on the toilet can affect hemorrhoids differently. Some hemorrhoids flare up close to the anal opening (external), while other flare-ups occur deeper inside the rectum (internal).
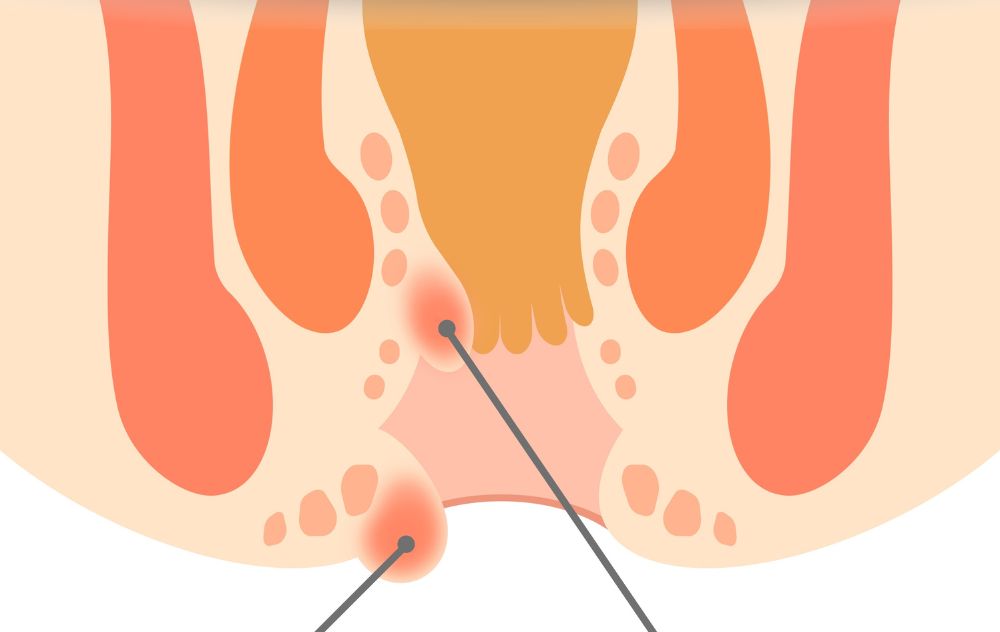
External hemorrhoids
External hemorrhoids are usually felt as a painful lump near the opening of the anus. They can be treated easily with over-the-counter topical creams or witch hazel. However, external hemorrhoids are more likely to develop a blood clot that can lead to intense pain and discomfort, requiring medical treatment to resolve it.
Internal Hemorrhoids (The USA Hemorrhoid Centers Focus)
Internal hemorrhoids are located inside the rectum. While they are not as painful as external hemorrhoids, they can bleed and leave a mark on toilet paper after wiping. The longer internal hemorrhoids are left untreated, the more swollen they become, eventually protruding from the anus (prolapse) during bowel movements.
Why It Matters
Internal hemorrhoids develop when the veins inside the rectum become swollen due to increased pressure and reduced blood flow. Prolonged sitting on the toilet — especially when distracted by a phone — can increase this pressure and delay normal blood return from the rectal area. Over time, repeated strain may weaken the supportive tissue that holds hemorrhoidal cushions in place, increasing the risk of bleeding or prolapse.
Because internal hemorrhoids are not always painful, many people ignore early warning signs such as light bleeding during bowel movements. Addressing the habits that contribute to this pressure — such as limiting time on the toilet — can help reduce flare-ups and prevent symptoms from progressing.
How Long Should You Sit on the Toilet?

To maintain healthy vein function and prevent hemorrhoid flare-ups, brevity is key. Specialists recommend limiting your time to five minutes or less; minimizing the duration of sitting reduces the prolonged pressure that triggers vein inflammation.
However, that does not mean you should strain during a bowel movement to avoid prolonged sitting on the toilet. Straining can also add pressure on the rectal veins and worsen hemorrhoid flare-ups.
Four Bathroom Habits that Protect Your Vascular Health

Aside from limiting the amount of time spent on the toilet, other habits to protect you from hemorrhoid flare-ups include:
- The 5-Minute Rule: If a bowel movement does not occur within five minutes, it is best to exit the bathroom and try again later. Prolonged sitting creates unnecessary gravitational pressure on the rectal veins.
- Establish a Device-Free Zone: To avoid “mindless scrolling” that leads to overextended sitting, leave smartphones and tablets in another room. Removing digital distractions helps you stay mindful of the time spent.
- Optimize Pelvic Alignment: Using a small footstool to elevate your knees (mimicking a squatting position) helps straighten the anorectal angle. This anatomical alignment allows for an easier passing with significantly less straining.
- Prioritize Hydration and Fiber: A diet rich in fiber paired with adequate water intake ensures softer stools. This is the most effective way to prevent forceful straining that causes rectal veins to become engorged.
What to Do If Hemorrhoid Symptoms Don’t Improve
For many patients with internal hemorrhoids, adopting new habits may not be enough to address the bleeding and swelling. If hemorrhoid symptoms persist for longer than a week, lead to a prolapse, or become chronic, it’s advised to seek a consultation with a hemorrhoid specialist.
USA Hemorrhoids Centers’ Approach to Hemorrhoid Relief
At USA Hemorrhoid Centers, we understand the toll chronic hemorrhoids can have on our patients. That’s why we offer a longer-lasting solution designed to reduce bleeding, swelling, and pressure from internal hemorrhoids.
We use a specialized approach to hemorrhoid care called hemorrhoid artery embolization (HAE). HAE is a minimally invasive treatment that reduces blood flow to internal hemorrhoids, causing the hemorrhoid to shrink and stop bleeding. The procedure helps alleviate hemorrhoid symptoms without a lengthy and painful recovery compared to traditional surgery.
HAE is performed as an outpatient procedure. Doctors use advanced imaging and catheters to precisely target the blood vessels contributing to hemorrhoid symptoms. Small particles are injected into these blood vessels, stopping the bleeding and causing the hemorrhoid to “deflate.” Following a short observation period, patients are discharged the same day with only a small adhesive bandage at the access site.
This procedure is often considered for patients with persistent internal hemorrhoids who haven’t found relief from lifestyle changes or previous medical procedures (e.g., rubber band ligation). A consultation helps determine whether this approach aligns with your symptoms and severity.
We are a trusted network of physicians who have helped many patients find relief from chronic hemorrhoids. Our physicians, many of whom are board-certified, are experts in the field of hemorrhoid care. They offer comprehensive evaluations to determine the next best steps for patients seeking relief.
If your “toilet scrolling” is causing your hemorrhoids to flare up, we are ready to help. Schedule a consultation online today or call (855) 805-4247 to learn more.
Source
- Ramprasad et al. 2025, “Smartphone use on the toilet and the risk of hemorrhoids”